GRID VIEW
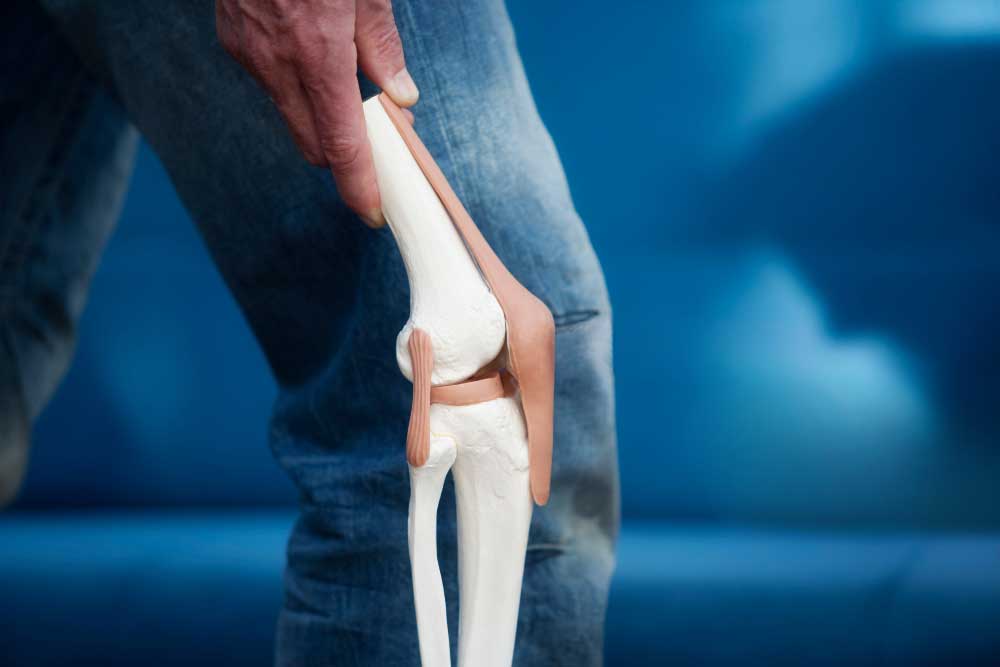
Old houses have creaky doors, and old bodies have creaky joints. Both are caused by the degradation of the joints. With doors, the lubrication from the hinges may have degraded, or the hinge may be out of alignment, causing the grinding of metal on metal. Our joints, including knees, are similar. The joints degrade, often from misalignment, causing pain and deformation. Unfortunately, we can’t pick up a replacement knee at the local hardware store. The most common condition causing joint degradation is osteoarthritis (OA). It affects around 20% of the global population, 500 million people. At its most basic, osteoarthritis is when joints start breaking down. It can affect different joints, but the knees are the most likely to be affected. Cartilage, the strong and flexible tissue that protects your joints and bones, breaks down in osteoarthritis. This causes joint pain, swelling, and loss of function (including range of motion) for the affected joint and may exacerbate comorbidities like diabetes and heart trouble. Women are more likely than men to have osteoarthritis and tend to have more severe symptoms. One major risk factor is obesity, which puts extra stress on joints like the knees and hips. They say age is just a number, but it is also a significant risk factor for OA. The risk of osteoarthritis peaks in a person’s ’60s. The incidence of osteoarthritis has more than doubled in the last 30 years, largely due to the aging global population. A big danger of OA is physical damage caused to the joint affected. This is called a biomechanical abnormality and could be due to a joint that is misaligned or has suffered prolonged abuse. Other risk factors for developing OA include metabolic syndrome, genetics, and trauma, such as torn ligaments. So what causes osteoarthritis? A lot of things! Cartilage is broken down, but many things may cause this. Outside of the joint, changes in bone, ligament, and muscle can cause stress or degradation. Inside the joint, inflammation, and cell death can lead to failure of the support structures. Inside joints are chondrocytes, the only type of cell in healthy cartilage. They normally spend their whole lives building and maintaining cartilage. They are so dedicated to their job that they become embedded in the structure of cartilage and die in place. With osteoarthritis, stressors (including the risk factors above) can cause chondrocytes to lament the poor work/life balance and start acting irrationally. Some chondrocytes degrade and stop supporting the cartilage (often by dying), and some go into overdrive, becoming larger and further destabilizing our cartilage structure. This causes the cartilage to shrink, and bones can start grinding against each other resulting in joint degradation. This is very painful and can reduce the quality of life dramatically. What can be done? One of the most important steps is to stop biomechanical abnormalities. Physiotherapy may help fix misalignments. Weight loss, lifestyle changes, and assistive walking devices can help reduce stress on joints. Surgery may be needed to replace or rebuild joints. Unfortunately, there are no approved medications that can cure osteoarthritis. Some anti-inflammatory medications may provide some relief, and are often prescribed. Luckily, the future is looking bright. Researchers are looking at new ways to target osteoarthritis, including next-generation anti-inflammatory medications, metabolic therapies, and even therapies that may rebuild cartilage through medication! In the future, we might not need to pick up a new knee at the hardware store, we might be able to build a new one on-site! Staff Writer / Editor Benton Lowey-Ball, BS, BFA
References: Goldring, M. B., & Otero, M. (2011). Inflammation in osteoarthritis. Current opinion in rheumatology, 23(5), 471. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3937875/ Gu, Y. T., Chen, J., Meng, Z. L., Ge, W. Y., Bian, Y. Y., Cheng, S. W., … & Peng, L. (2017). Research progress on osteoarthritis treatment mechanisms. Biomedicine & Pharmacotherapy, 93, 1246-1252. https://doi.org/10.1016/j.biopha.2017.07.034 He, Y., Li, Z., Alexander, P. G., Ocasio-Nieves, B. D., Yocum, L., Lin, H., & Tuan, R. S. (2020). Pathogenesis of osteoarthritis: risk factors, regulatory pathways in chondrocytes, and experimental models. Biology, 9(8), 194. https://www.mdpi.com/2079-7737/9/8/194 Poole, A. R., Guilak, F., & Abramson, S. B. (2007). Etiopathogenesis of osteoarthritis. Osteoarthritis: diagnosis and medical/surgical management, 4, 27-49. https://www.sciencedirect.com/science/article/abs/pii/S0025712508001223?via%3Dihub Long, H., Liu, Q., Yin, H., Wang, K., Diao, N., Zhang, Y., … & Guo, A. (2022). Prevalence trends of site‐specific osteoarthritis from 1990 to 2019: findings from the Global Burden of Disease Study 2019. Arthritis & Rheumatology, 74(7), 1172-1183. https://doi.org/10.1002/art.42089
Scroll down to listen to this article.
Listen to the article here:
Healthy eating and exercise can help with not only your waistline but also cardiometabolic health. Carrying around extra fat can negatively affect your whole body; some areas of concern include the liver, heart, and joints. Although many people can maintain a healthy diet and exercise routine to keep the weight off, some folks need extra help with medication.
The liver is the largest organ inside your body and is integral in filtering harmful substances from your blood. When too much fat builds up in your liver, this is called fatty liver disease. This can progress to damaging and scarring of the liver. The scaring can ultimately lead to liver failure. Lifestyle changes, like healthy eating and exercise, are currently the only treatments for fatty liver disease, although many clinical trials are currently looking for a safe and effective therapy.
Heart disease remains the world’s leading killer. While extra fat itself does not directly cause heart attacks, it leads to other causes that can. High cholesterol, high blood pressure, and diabetes are among those that build up plaque in the arteries leading to heart attacks. ENCORE Research Group offices have many clinical trials in these areas!
Being overweight can affect your joints by raising your risk of developing osteoarthritis. The extra weight puts additional stress on your weight-bearing joints, such as your knees, which can cause additional wear and tear. Additionally, inflammation associated with weight gain might contribute to problems in other joints such as the hands.
For the folks who need more than just a healthy diet and exercise to help with medical conditions, the good news is that many new cutting-edge treatments are being studied and are available to you. Call your local ENCORE Research Group office today to get involved in our research trials.
Sources:
heathline.com
health.clevelandclinic.org
health.harvard.edu
Writen by: Mike Mass, MD
Rheumatoid arthritis (RA) is an autoimmune disease that is localized in the joints but may also result in serious systemic symptoms. In the joints, RA begins in the lining tissue known as synovium. In RA inflammatory cells are stimulated in the synovium and release substances that will both activate other inflammatory cells and cause direct breakdown in the adjacent bone. If this inflammatory process is not interrupted it will immediately cause severe damage to the joint and, on occasion, other organs in the body.
Until recently, the only treatments available helped the symptoms of inflammation, such as pain and tenderness, but did little to stop the destructive process. The first drug that had some limited benefit was gold salts, but it was toxic and had to be monitored carefully. Low doses of a cancer drug (Methotrexate) were tried and proved effective in treating the symptoms of inflammation and also slowed down the destructive process in many patients and was a mainstay of therapy until the last decade.
As the understanding of the autoimmune abnormality increased, various substances released from inflammatory cells were identified. Initially, the most promising of these was known as tumor necrosis factor (TNF). While in other studies it had affected some tumor growth, it was also found to be a major cause of damage in RA. A group of anti-TNF monoclonal antibodies is on the market and has proven to be quite effective in a large number of patients. The search has continued for other substances that will either modify the autoimmune response or inactivate substances that cause damaging inflammation. Recently another protein has been identified that is present in the synovium and when activated will initiate a whole range of responses that result in a proliferation of synovial cells which then go on to damage the joint. This particular substance is part of a larger group of proteins known as “Integrins.” It is hoped that by giving a monoclonal antibody directed against the particular integrin a major portion of damaging inflammation will be shut down. A clinical trial of this antibody just opened at Jacksonville Center for Clinical Research University Blvd. Office and we are currently seeking volunteers. Call today to see if you qualify! 904-730-0166
Joint pain is an ancient disease. Dinosaur skeletons, cavemen remains, and ancient Egyptian mummies all have evidence of it. In 1886 an English doctor named John Kent Spender coined the term “osteoarthritis” (OA) which led to the modern understanding of the disease.
To relieve the pain and suffering of OA, ancient healers tried various concoctions, some of which persist until today. . More than 2500 years ago, Egyptian physicians treated OA with ointments containing fat, oil, honey or bone marrow, often added to various dry ingredients such as: flour, baking soda, cumin and incense. 1 The father of medicine, Hippocrates, observed that “Swelling and joint pain, ulcers, those of a gouty nature and muscle strain are usually improved by cold water, which reduces swelling and eliminates the pain, as a moderate degree of numbness eliminates pain”. Another Greek physician named Dioscorides floated a less enduring idea. He recommended using ivy. This treatment proved less effective although the subsequent itching may have distracted patients from thinking about their joints.
Acupuncture, an effective therapy for some folks, is another ancient treatment that has remained virtually unchanged over many years. An older medicinal approach using willow bark leaves remains in use today. These leaves contain salicylic acid. An understanding of the benefits of salicyclic acid ultimately led to a breakthrough by a French chemist named, Charles Frederic Gerhardt. Gerhardt’s claim to fame involved the chemically synthesize of Aspirin or acetylsalicylic acid in 1897 that improved upon salicylic acid.
In more recent years, clinical research has helped to shed some light on this painful disease. Though there is no cure for OA, researchers have found many treatments to manage symptoms. Science has proven that physical activity is one of the most beneficial ways to manage OA. The CDC recommends exercises such as: brisk walking, bicycling, swimming and muscle strengthening activities. It’s important for you to get moving and keep moving! Losing weight can also help relieve additional stress on your weight bearing joints.
If older therapies haven’t worked for you or someone you know, there is always the promises of modern medicine. Thanks to years of clinical research there are some great medications available both over-the-counter and by prescription. Analgesics such as Tylenol, opioids (narcotics) and tramadol are pain relievers. Nonsteroidal anti-inflammatory drugs (NSAIDs) are the most common anti-inflammation medication. NSAIDs include: aspirin, ibuprofen, naproxen, and Celebrex. Corticosteroids are powerful anti-inflammatory medicines most notably given by injection in a doctor’s office. Hyaluronic acid naturally occurs in joint fluid, acting as a shock absorber and lubricant. Hyaluronic acid is given by injection in a doctor’s office.2 We don’t suggest using any treatments without first checking with your doctor!
The future for OA treatments looks bright. You can participate in the path to the future by participating in a clinical trial. We have many programs available at no charge. Please give us a call so we can see which program works best for you!