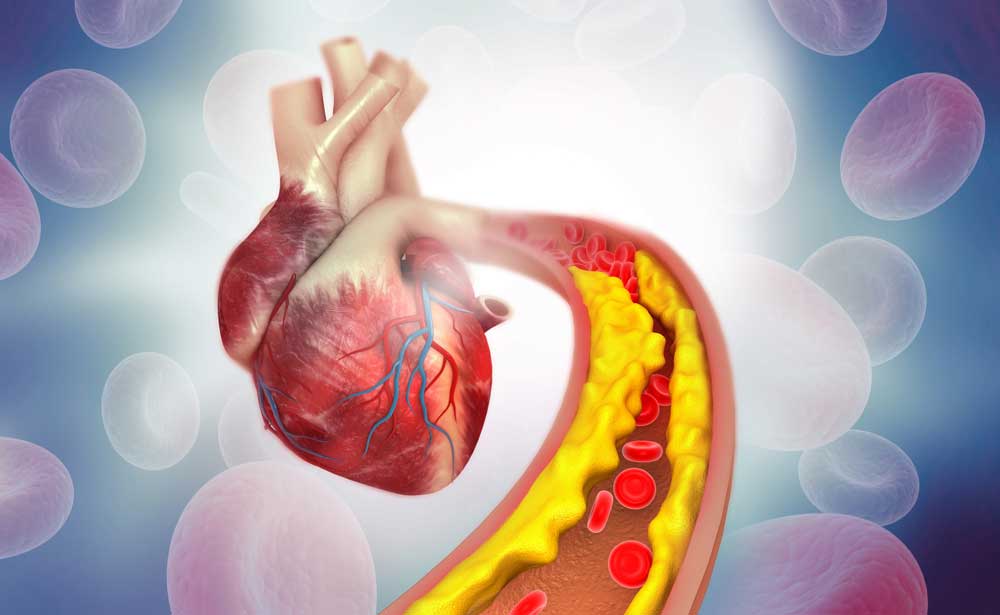
5 Things to Know about Lp(a) Lipoprotein(a), or Lp(a), is an independent risk factor for atherosclerotic cardiovascular disease. Cardiovascular disease is the leading cause of death in both men and women in the US and globally . You may have heard of LDL cholesterol, or “bad cholesterol,” as a risk factor for heart disease, but Lp(a) can be just as dangerous. Lp(a) flies under the radar of many physicians. This is because the awareness of Lp(a) is still very low, very little is understood about the protein and the treatment options are limited. What is LP(a)? Lp(a), pronounced “LP little a,” is a protein that is attached to LDL cholesterol. It is composed of an LDL-like particle, but it has a second protein coiled around it. Recent studies have shown that people born with elevated Lp(a) can be two to four times as likely to have a heart attack or serious cardiac related risk. Lp(a) is present in 20% of the population. What differentiates LP(a) from other heart disease risk factors? LP(a) is so unique because it is a completely genetic risk factor. Meaning, having an elevated LP(a) is almost entirely determined by the genes you inherit. There is no evidence that a healthy lifestyle will lower your Lp(a). However, that does not mean those with high levels shouldn’t practice healthy habits. Reducing other risk factors that are determined by quality of health can still reduce the overall risk of heart disease. Another risk factor that sets LP(a) apart is that it is an independent risk factor. It has been linked to heart disease in younger adults who are otherwise healthy and have no prior cardiovascular risks. Elevated LP(a) has affected the lives of many who are otherwise healthy. For example, Tennis legend Arthur Ashe, who had his first heart attack at age 36. Bob Harper, a celebrity fitness trainer was also affected and nearly died of a heart attack at age 52. Who should be tested for Lp(a)? Studies show that there is a higher risk of a cardiovascular event if Lp(a) levels start to rise above 30 mg/dl. There is an even greater risk at levels 50 mg/dl and higher. There are an estimated one in seven people at or above this threshold. If you’ve had a cardiac event but your cholesterol levels are normal, or you have a family member with heart disease at an early age, have a cardiovascular event despite normal lipid levels, have a family history of Lp(a), or have aortic valvular disease at an early age then you should get tested for Lp(a). As mentioned, Lp(a) is a genetically mediated risk factor. “This means it runs in families,” Albert Lopez, MD, DO, FASPC, internal physician and lipid specialist in Jacksonville, FL says. “Those individuals that have it, you have a 50% chance of giving to your children.” Dr. Lopez believes there should be cascade screening, meaning asking family members if they have it and then getting tested. No FDA approved remedies for Lp(a) Currently there are no FDA approved remedies for elevated Lp(a). Statins, a widely known and used therapy that lowers LDL cholesterol does not reduce Lp(a) and has been shown to sometimes result in a slight increase. One therapy that has been shown to work is asphersis. This process filters a patient’s blood by circulating it through a machine and removing Lp(a) particles. However, this process is reserved for high-risk patients because it is extremely expensive, requires weekly visits and involves risks. After stopping apheresis, the Lp(a) levels begin to rise again. New Advancements in Science regarding Lp(a) Luckily, there are new drugs on the horizon that could potentially help those suffering from elevated Lp(a) levels. “What is exciting is that we are in totally nerd, sci-fi treatments now,” Dr. Lopez says. “We can actually stop your genes from making this protein by using a little snip that crinkles it up and doesnt let it read.” In other words, new studies are using gene silencing techniques to achieve a large and durable reduction of Lp(a). These therapies and medicines are still in clinical trials now. ENCORE Research group is conducting research studies for people with elevated Lp(a) in hopes to find a drug that will lower Lp(a) levels. It is up to the public to participate in these research studies to help those suffering from elevated Lp(a) levels.
GRID VIEW
For some patients, managing cholesterol creates a challenge. Statins are a safe and standard treatment but many people have very high levels of cholesterol that require more than statin drugs alone. Others cannot easily tolerate statins. Nonetheless, treating cholesterol saves lives and avoids heart attacks and strokes. Thankfully, the future is here with new breakthroughs that can change the way we maintain healthy cholesterol levels due to continued research and clinical trial participants. We outline some of these exciting technologies below. Antisense oligonucleotides (ASOs) are short, synthetic single stranded fragments of RNA that can reduce, restore or modify protein expression. ASOs have been designed specifically to target high levels of LDL (bad cholesterol) in the bloodstream in a different way than current medications. Firstly, ASOs targets the source of the disease resulting in a higher chance of success compared to therapies targeting downstream pathways. Secondly, ASOs are not metabolized by cytochrome P450 as most other drugs are. This significantly reduces the chance of one drug interacting with another drug in the body which could potentially cause more harm than good. Small interfering RNA (SiRNAs) are another type of RNA therapy that is being used in clinical trials to reduce the risks of cardiovascular disease. Unlike ASOs which are single-stranded oligodeoxynucleotides, siRNAs are double-stranded RNA molecules. SiRNAs are used in the silencing of disease-causing genes, in this case the genes involved in creating cardiovascular diseases, and it has made great progress. Adnectins are a class of drugs used to target proteins. Adnectins can be rapidly developed to bind proteins or other necessary targets. Currently, adnectins are being used in clinical trials to bind with a human protein called PCSK9. This binding blocks the interactions between PCSK9 and LDL (bad cholesterol) receptors. As a result, the levels of LDL cholesterol in the body are lowered. These technologies hold the potential to not only better manage cholesterol levels and thereby reducing heart attack and stroke risk, but many other conditions as well. Source: US National Library of Medicine
National Institutes of Health
The old saying goes: Men are from Mars and Women are from Venus. This exaggeration is- well… an exaggeration, but there are some differences between male and female heart health that causes an inkling of truth to shine out through the expression. The most common kind of heart disease, among both men and women, is coronary artery disease. Coronary artery disease is caused when cholesterol plaque is built up inside the arteries, and if left untreated coronary artery disease can obstruct blood flow to the heart muscle and lead to a heart attack.
When experiencing a heart attack, the individual will usually experience chest pain, shortness of breath, and pain in their left arm, but these symptoms are not universal. Remember when we were talking about the differences between men and women? Women are more likely to experience uncommon heart attack symptoms than men are! These symptoms can include indigestion, pain in both arms, unusual fatigue and abdominal discomfort. Physicians are still uncertain why women are more likely to experience unusual symptoms. There are some theories about hormonal changes and the difference in valve and vessel sizes, but for the most part it is still unknown.
Lowering your risk of a heart attack, however, is not a mystery. Research shows staying active, eating healthy, and monitoring your blood pressure and cholesterol levels regularly leads to decreased cardiovascular risk. Research also shows that individuals involved in clinical research have better health care outcomes than those who are not.
We are currently enrolling in studies that may help you lower important factors like elevated triglycerides and cholesterol which may help lower your risk of cardiovascular events.
References:
https://www.hopkinsmedicine.org/heart_vascular_institute/centers_excellence/womens_cardiovascular_health_center/patient_information/health_topics/menopause_cardiovascular_system.html
https://www.lahey.org/article/differences-between-mens-and-womens-hearts/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3018605/
https://www.clinicaltrials.gov
What causes a heart attack?
A heart attack (myocardial infarction) means that blood flow to the heart muscle has been decreased enough to cause damage to the heart muscle. Some causes of blocked blood flow include blood clots, cholesterol build up, and rupture of plaque within the blood vessel. For those who have already suffered a heart attack, it is important to reduce the risk of recurrent attacks. Research has shown that there are several steps that can be taken to help reduce the risk of recurrent heart attacks.
Proven things you can do to prevent heart attacks
- Lower cholesterol
- Lower triglycerides
- Lower blood pressure
- Stop smoking and avoid secondhand smoke
- Eat fish
- Increase physical activity as allowed by your doctor. Inactive people have nearly twice the risk of heart disease as those who are active.
- Talk with your doctor about medicines that can decrease blood clotting
Medications that can reduce risk of heart attack
- Cholesterol lowering medication, which include statins and non-statins
- Triglyceride lowering medications
- Medications that decrease inflammation
Current research is underway to study improving health after a heart attack
- Weight loss: Heart attack is three times higher in those who are obese than in those who are lean.
- New medications for those with unique cholesterol metabolizing problems.
- Anti-inflammatory medications targeting inflammation in blood vessels.
At ENCORE Research Group we have clinical research studies for many of the risk factors mentioned above. Participating in a research study can help keep you motivated on your journey to better health. If you are interested in participating in any of our research studies, call your local office today!
The heart is vital (literally), so it’s important to keep it in tip-top shape! The rest of the body depends on the heart to deliver blood and oxygen to all its cells and organs. If the heart becomes damaged, it can lead to what is known as heart failure. Keeping your heart healthy not only involves proper diet and exercise, but also involves making sure conditions that can cause heart damage are properly managed.
Some conditions that can damage the heart are:
- cardiomyopathy
- coronary artery disease
- diabetes
- heart attacks
- high blood pressure
During heart failure the heart is unable to pump blood effectively enough to meet the body’s demands. Because the heart cannot fulfill its primary duty, it will try to compensate by enlarging itself, increasing muscle mass or pumping faster. The body can also react by narrowing blood vessels and diverting blood away from less important tissues and organs. As heart failure worsens the compensations and symptoms begin to show.
Common symptoms of heart failure include: shortness of breath, fatigue, coughing, racing heart, excessive tiredness, loss of appetite, and chest pain. Risk factors for developing heart failure include diabetes, poorly controlled high blood pressure, high cholesterol, or family history of heart failure. If you think you might have symptoms of heart failure, it’s important to speak with your doctor as soon as possible.
There are about 5.7 million adults in the United States who have heart failure and it’s the leading cause of death in diabetics. In most cases, heart failure cannot be reversed once diagnosed. However, researchers are continuing to study ways to reverse heart failure as well as new and better ways to treat it. Currently, many of our ENCORE research sites have new heart failure research studies enrolling. If you or someone you know has heart failure, and are interested in participating, call our office to find out more!
Three New Breakthroughs in Heart Disease
Heart Disease is a general term for heart conditions that negatively impact the heart’s ability to perform its vital functions. On average 1 in 4 American deaths each year are due to heart disease. Fortunately, each year new discoveries are made that allow us to treat heart disease more successfully. Here are three of the latest discoveries.
- Dialysis for Heart Failure?
One of the symptoms of heart failure is fluid retention, which can lead to kidney
problems. Diuretics are currently the standard treatment for fluid retention, however there is a new treatment where a catheter in inserted through the neck so that it surrounds a major lymphatic vessel. The excess fluid is removed from the lymphatic system and then pumped back into the circulatory system where it is removed by the kidneys. This new treatment avoids some of the negative side effects of oral diuretics such as low blood pressure and decreased kidney function.
2. Beta Blockers: Old dog, new tricks?
A new study at York University in Toronto has analyzed the effect of beta blockers on
coronary gene expression in patients with heart failure. Researchers found that beta blockers “largely reverse the pathological pattern of gene expression observed in heart failure.” More research is needed to determine whether beta blockers can be used to protect against heart failure.
3. Tick saliva saving lives?
While ticks are often the subject of nightmares researchers now believe they can lead to a dream solution for myocarditis, heart attack and stroke. Ticks use proteins called ‘evasins’ to escape their host’s detection by blocking the host’s inflammatory response. Researchers are now isolating these evasins in a ‘bug to drug’ formula. Hopefully these drugs will be able treat a variety of inflammatory diseases.
At ENCORE Research Group we conduct cutting edge research similar to those seen above. While we do not have any ‘bug to drug’ studies at this time, we do have a heart failure study involving a new use for an already FDA approved medication. If you are interested in learning more about our current studies visit our “Enrolling Studies” tab at the top of the page.
If you have high cholesterol you may dread going to your doctor, especially if they are going to complete a cholesterol blood test. You know they prescribed a statin, but the muscle cramping you experience after taking it just isn’t worth it. How do you tell your doctor that the medication they prescribed just isn’t working for you? You are not alone, and there are options available for you.
We all know that having excess cholesterol in our blood is a bad thing, but why is it so bad? High cholesterol has often been called ‘The Silent Killer’. In fact, according to the CDC heart disease is responsible for 1 in 4 American deaths every year.[1] High cholesterol is known to cause plaque formation in arteries, constricting blood flow to vital organs in your body. Even worse, cholesterol plaques can become dislodged from the walls of the arteries potentially causing blood clots. Both heart attacks and strokes can be caused by plaques reaching the heart or brain respectively. If lifestyle changes such as a good diet and exercise can’t bring down your cholesterol numbers, you may need a medication. The most common cholesterol lowering medications to date are statins such as Crestor, Lipitor, or Zocor. These medicines have been life saving for many people that can tolerate them. However, some people are intolerant to statins and will experience side effects such as painful muscle cramps, inflammation and more.
If you are allergic to or can’t handle statins what can you do? It is crucial to keep your cholesterol levels down, lowering your risk for a heart attack and stroke. You may try one of the medications already on the market for people with statin intolerance such as Zetia, Juxtapid and Repatha. However, each of these drugs have their own risks. Zetia can cause symptoms similar to those caused by statins. Juxtapid, a newer medication, has been found to significantly reduce LDL bad cholesterol by 40-50%. Sadly, it also caused diarrhea, nausea, vomiting or abdominal pain in 28% of patients.[2] In 2015 the FDA approved Repatha, a new class of drug called a PCSK9 inhibitor that is very successful in lowering LDL. Unfortunately, due to the cost of development and production the annual cost is around $14,000 dollars making it unaffordable for most people.
If you’ve had trouble taking statins in the past you may be asking “what do I do now”? Many of our participants are looking for alternative treatments or want to be part of cutting edge research. I encourage you to check out the cholesterol research studies we are conducting at many of our research centers. You may qualify for a new oral medication or to receive PCSK9 in an upcoming study! The medicines being researched for people who cannot take statins may significantly alter the future of cardiovascular disease. We need your help to bring these new medications to market!
References:
[1] “Heart Disease Fact Sheet.” Centers for Disease Control and Prevention. Centers for Disease Control and Prevention, 16 June 2016. Web. 27 Apr. 2017.
[2] Orrange, Sharon, MD. “Finally, a Non-Statin Cholesterol Medication That Works: Introducing Juxtapid.” The GoodRx Prescription Savings Blog. N.p., 06 June 2014. Web. 27 Apr. 2017.