GRID VIEW
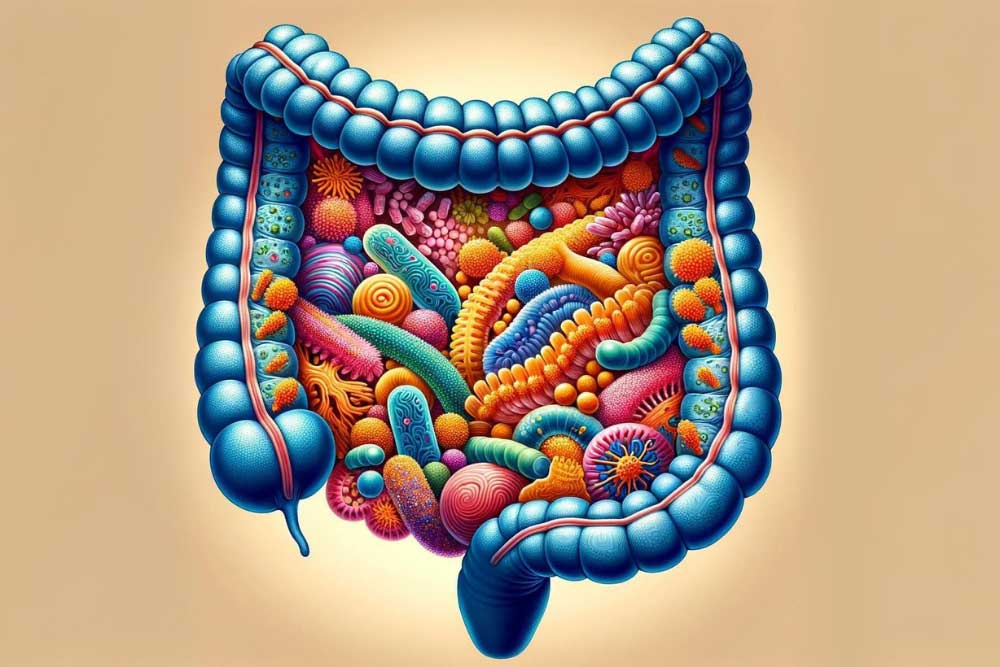
When we think of an animal, we generally think of a single creature with a unique DNA code. A human starts as a single fertilized egg cell with the combined genetic code from our parents. By the time we’re walking and talking, however, we’ve already transformed into a superorganism. If you were to count the number of cells that make you up, only half would be human. Mature red blood cells lack a nucleus, so if we count only cells with nuclei, we’re only about 10% human. Going further, if we count all the genetic material in our body, only about 1% of it is human. Genetically, we’re 99% nonhuman. So then, what are we? Bacteria. We’re primarily bacteria. These bacteria live with us our whole lives. They live on our skin, in our hair, on our eyelashes, and in our gut. The bacteria that live in the digestive tract, along with the relatively minuscule amounts of viruses, archaea, and yeasts, make up the gut microbiome. The gut microbiome is incredible. It establishes itself until around age two. It changes in response to the food we eat, diseases we get, medications we take (especially antibiotics), and our hygiene. We eat around 60 tons of food in our lives, and the gut microbiome has a hand in all of it. We usually think of bacteria (and viruses, etc) as parasitic (doing damage). The reality is the gut microbiome is truly symbiotic, we need it as much as it needs us. The gut microbiome performs many tasks for us. It shapes the human cells and the mucus that lines our gut, strengthening it. It protects us from infections, keeps our cells together in a tight barrier, and communicates with the immune system. Microbiome cells outcompete other, destructive bacteria. They can also release bacteriocins (bacteria-targeting toxins) that destroy dangerous bacteria. The microbiome is so stellar it helps us even when it’s just eating. The gut microbiome breaks down foods we can’t process, like dietary fiber. Through the process of fermentation, it uses this food to make vitamins, minerals, etc. As an example: we can’t make vitamin B12 at all in our cells; we rely on microorganisms to make it for us! Finally, the gut microbiome makes short-chain fatty acids. Short-chain fatty acids are the primary energy source for the human cells that line the intestine. They also increase insulin sensitivity and mediate immune regulation, inflammation, and other body processes. Unfortunately, the gut microbiome can get out of whack, and issues like ulcerative colitis – an inflammatory bowel disease – can occur. To understand what can go wrong, let’s first investigate a healthy gut microbiome. The colony of colon bacteria is unique in everyone. A healthy microbiome has three qualities: high diversity, high richness, and high stability. Diversity is just what it sounds like: the total number of different species present. Richness is the balance between species; having roughly equivalent numbers of bacteria from each. Stability is the consistency of finding the same types and numbers of organisms over time. So what does a disruption in the balance of the gut microbiome look like? Loss of diversity, overgrowth of some types of organisms, and changes to the composition of the gut microbiome over time. The degradation of diversity, richness, or stability is called dysbiosis. One cause of dysbiosis is antibiotics. They are designed to kill bacteria, which is bad news for the gut bacteria. Antibiotics frequently lead to a redistribution of gut microbiota. Other things that can cause dysbiosis include hygiene, infection, and smoking. The most important, however, is diet. All of the food we eat travels through the gut. In the western world, our diets aren’t always built to cultivate a healthy gut microbiome. Much of our food is built for shelf stability and is made using enzymes or chemicals instead of bacteria. We tend to eat more animal fats and proteins and fewer plant fibers than indigenous populations. To top this off, we eat refined sugar. Like, a LOT of refined sugar. Around 50 to 100 pounds of refined sugar per year. I’m not a nutrition expert, but I am a cookie expert, and that’s way too many cookies. When the microbiome is in a state of dysbiosis, it can’t perform its helpful functions. The mucus layer is reduced, bacteria can’t interact with the immune and inflammation systems, and the gut is more permeable to undesirable substances. On top of this, short-chain fatty acid production decreases, making it more difficult for the human cells lining the gut. This loss of function is linked to diseases like ulcerative colitis. The exact causes of ulcerative colitis are unknown, but scientists think it is related to the gut microbiome. Ulcerative colitis is a chronic inflammatory disease with periods of high and low activity. Inflammation leads to painful ulcers along the colon and rectum. So what can we do when the gut is out of whack? This is still a relatively new area of research, so there are many questions we have to answer. Our best solutions so far are food and feces. The importance of food to the gut microbiome should be obvious by now. Foods high in dietary fibers from plants are needed for gut bacteria to survive and thrive. The role of bacteria derived from human feces is still being developed. Fecal transplantation is a fascinating, but not-for-the-dinner-table line of study. The basic idea is that doctors would transfer some of the gut microbiome from a healthy person to a sick one, perhaps someone with ulcerative colitis. These bacteria would hopefully colonize and outcompete whatever is disrupting the sick microbiome, restoring diversity, richness, and stability. Focusing on the symbiotic relationship we share with our individual microbiome will revolutionize our approach to healthcare. Clinical trials may pave the way forward for treatments that support our human cells and our microbiome, nurturing the microbial communities vital to our survival and well-being as a superorganism. Also, don’t forget to eat your veggies. Staff Writer / Editor Benton Lowey-Ball, BS, BFA
References: Bengmark, S. (1998). Ecological control of the gastrointestinal tract. The role of probiotic flora. Gut, 42(1), 2-7. https://doi.org/10.1136/gut.42.1.2 Fan, Y., & Pedersen, O. (2021). Gut microbiota in human metabolic health and disease. Nature Reviews Microbiology, 19(1), 55-71. https://doi.org/10.1038/s41579-020-0433-9 Gomaa, E. Z. (2020). Human gut microbiota/microbiome in health and diseases: a review. Antonie Van Leeuwenhoek, 113(12), 2019-2040. https://link.springer.com/article/10.1007/s10482-020-01474-7 LeBlanc, J. F., Segal, J. P., de Campos Braz, L. M., & Hart, A. L. (2021). The microbiome as a therapy in pouchitis and ulcerative colitis. Nutrients, 13(6), 1780. https://doi.org/10.3390/nu13061780 Sender, R., Fuchs, S., & Milo, R. (2016). Revised estimates for the number of human and bacteria cells in the body. PLoS biology, 14(8), e1002533. https://doi.org/10.1371/journal.pbio.1002533 Świrkosz, G., Szczygieł, A., Logoń, K., Wrześniewska, M., & Gomułka, K. (2023). The Role of the Microbiome in the Pathogenesis and Treatment of Ulcerative Colitis—A Literature Review. Biomedicines, 11(12), 3144. https://doi.org/10.3390/biomedicines11123144 Tan, J., McKenzie, C., Potamitis, M., Thorburn, A. N., Mackay, C. R., & Macia, L. (2014). The role of short-chain fatty acids in health and disease. Advances in immunology, 121, 91-119. https://doi.org/10.1016/b978-0-12-800100-4.00003-9 The Human Microbiome Project Consortium. (2021). Structure, function and diversity of the healthy human microbiome. Nature 486, 207–214. https://www.nature.com/articles/nature11234 Thursby, E., & Juge, N. (2017). Introduction to the human gut microbiota. Biochemical journal, 474(11), 1823-1836. https://portlandpress.com/biochemj/article/474/11/1823/49429 Xiong, R. G., Zhou, D. D., Wu, S. X., Huang, S. Y., Saimaiti, A., Yang, Z. J., … & Li, H. B. (2022). Health benefits and side effects of short-chain fatty acids. Foods, 11(18), 2863. https://doi.org/10.3390%2Ffoods11182863 Young, V. B., & Schmidt, T. M. (2008). Overview of the gastrointestinal microbiota. Advances in experimental medicine and biology, 635, 29–40. https://doi.org/10.1007/978-0-387-09550-9_3
Listen to the article here:
High blood pressure is amazingly prevalent, affecting nearly half of all Americans. It’s a major risk factor for heart attack, stroke, kidney failure, eye damage, and more. Unfortunately, this condition remains highly prevalent despite the numerous medications designed to treat it. For many patients, adhering to medications can be difficult, and for others, some medicines are not effective in reducing blood pressure levels. But what if there were a way to lower blood pressure at the source, the heart? First, let’s examine how the heart relates to blood pressure. It might seem obvious, but it’s actually quite complex. The heart draws blood in and pushes it out with each beat. The amount of blood pumped is called the stroke volume. A good stroke volume helps to ensure the heart has enough blood pressure to deliver oxygen throughout the body. A healthy heart will pump out around 50-70% of the total volume of blood. This means there remains some unpumped fluid in the heart chambers after pumping is complete. When the next heartbeat comes, the heart muscle has to stretch enough to accommodate this unpumped blood. This extra blood increases our blood pressure because of the Frank-Starling law of the heart. The Frank-Starling law of the heart is over 100 years old and states that the amount our heart muscles stretch before pumping scales with the force they deliver when pumping. Think of a rubber band. If you stretch it a little, it’ll flop back in place. If you stretch a rubber band a lot, almost to its breaking point, it’ll snap back so hard as to leave a welt on your skin. The heart is similar; extra blood in the heart before pumping increases the pressure of each beat and maintains our blood pressure. If there were a way to lower the amount of blood in the chamber after beating, it follows that blood pressure may be lowered. Note that just the pressure would be lowered. The stroke volume would (ideally) remain the same. But how could we do this? For most people, we don’t have any way of convincing the heart to empty more effectively. For a select few, however, the hardware may already be in place. Pacemakers are amazing technology that has helped countless people whose hearts aren’t working properly. Over a million pacemakers are implanted every year worldwide and help people with arrhythmias. Arrhythmias are conditions that involve irregular heartbeat. Pacemakers are surgically implanted devices that send small amounts of electricity where they are needed in the heart. Heart muscles are triggered by this little zap and beat in response to it. Pacemaker rhythms can be customized for several types of conditions, and can even be programmed after being implanted to adapt to changing patient conditions. This is where a pacemaker’s ability to help with high blood pressure is theorized. By customizing how a pacemaker fires, it is possible to cause the heart to release more of its contents and lower the amount of blood remaining in the heart before pumping. According to the Frank-Starling law of the heart, this should result in lower blood pressure (indeed, early clinical trials show this to be the case). Finally, we have to make sure changes to our blood pressure bypass the sympathetic nervous system. This pathway, also called the “fight or flight” pathway, helps ensure the body is awake, alert, and alive. Integral to this system are receptors that sense our blood pressure. If the sympathetic nervous system senses a prolonged drop in blood pressure, it kicks in to correct this. This is a critical system that keeps us from constantly fainting but can be problematic when trying to lower blood pressure. A clever workaround being investigated is to have a pacemaker lower the blood pressure intermittently. It runs the chamber-emptying algorithm for short periods of time. This may help bypass our sympathetic nervous responses. If clinical trials bear out, pacemakers may be able to change not just the pace of the heart, but the pressure too! Staff Writer / Editor Benton Lowey-Ball, BS, BFA
References: Centers for Disease Control and Prevention. (2023). Facts about hypertension. U.S. Department of Health & Human Services. https://www.cdc.gov/bloodpressure/facts.htm Mond, H. G., & Proclemer, A. (2011). The 11th world survey of cardiac pacing and implantable cardioverter-defibrillators: calendar year 2009–a World Society of Arrhythmia’s project. Pacing and clinical electrophysiology : PACE, 34(8), 1013–1027. https://doi.org/10.1111/j.1540-8159.2011.03150.x Kalarus, Z., Merkely, B., Neužil, P., Grabowski, M., Mitkowski, P., Marinskis, G., … & Kuck, K. H. (2021). Pacemaker‐Based Cardiac Neuromodulation Therapy in Patients With Hypertension: A Pilot Study. Journal of the American Heart Association, 10(16), e020492. https://www.ahajournals.org/doi/full/10.1161/JAHA.120.020492 Mitchell, L.B. (2023). Cardiac pacemakers. Merck Manual, Professional Version. https://www.merckmanuals.com/professional/cardiovascular-disorders/overview-of-arrhythmias-and-conduction-disorders/cardiac-pacemakers Neuzil, P., Merkely, B., Erglis, A., Marinskis, G., de Groot, J. R., Schmidinger, H., … & Kuck, K. H. (2017). Pacemaker‐mediated programmable hypertension control therapy. Journal of the American Heart Association, 6(12), e006974. https://www.ahajournals.org/doi/full/10.1161/JAHA.117.006974 Sequeira, V., & van der Velden, J. (2015). Historical perspective on heart function: the Frank–Starling Law. Biophysical reviews, 7, 421-447. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5418489
Listen to the article here:
I recently went to a dessert party. That’s a party where everyone brings a dessert. I, naturally, arrived with cookies while others brought cakes and pies. Surprisingly, there was one attendee who presented a bowl of berries, another who showcased a sweet potato casserole, and a third who simply brought avocado with a dash of salt. Do these all count as desserts? What is a dessert? A word that was clear at the outset was quickly confusing in how broad it was. Unfortunately, that confusion can also happen with medical terms. Take cardiovascular disease. It’s got something to do with the heart, but sometimes it includes strokes in the brain. So what is cardiovascular disease? “Cardiovascular” is a word made of two component parts: cardio- means “heart” and vascular indicates blood vessels. Together, cardiovascular disease is that which affects the heart and/or blood vessels. The heart and blood vessels carry oxygen to the cells and keep them alive. Since we’re made of cells, keeping them alive is pretty important. Therefore, the heart and blood vessels are also quite important, and cardiovascular disease can be dangerous if not managed. Cardiovascular disease is more common than apple pie in the United States. Data from the CDC show that nearly HALF of adults over 20 have some form of cardiovascular disease. With a prevalence that high, it’s no surprise that cardiovascular disease is the leading cause of death in America and around the world. Unfortunately, as noted above, the exact definition of “cardiovascular disease” is very broad. In researching this article you are currently reading, I consulted the World Health Organization, the American Heart Association, and the National Institute of Health (part of the CDC). These organizations listed the various diseases included in cardiovascular disease, and only agreed on two conditions: Other diseases that at least two agreed on include: Though all these diseases may seem different, they are all part of the same system. Narrow blood vessels to the heart or brain cause oxygen loss. This narrowing can be caused by plaque formed when cholesterol lodges in the vessel wall. If some of this plaque dislodges, it can lead to heart attacks and strokes. Irregular heartbeats and heart attacks can lower the amount of blood (and oxygen!) delivered around the body. Hypertension stresses the whole system and can lead to heart attack, stroke, and damage to other organs like the kidneys. Additionally, they may have similar risk factors, outcomes, and treatments. There is a genetic component to cardiovascular disease. This is evident with congenital heart defects, which occur during development. It is also evident looking at who is at risk of developing cardiovascular disease. African Americans are at the highest risk, while people who identify as Hispanic have the lowest risk. Big modifiable risks include cholesterol, smoking, and hypertension (which is itself a form of cardiovascular disease!). Other risks include diabetes, being overweight, poor diet, low exercise, alcohol consumption, and low sleep. Research is ongoing into the cycle of mental health and cardiovascular disease as well. Mood and anxiety disorders, PTSD, and chronic stress can cause direct damage to the cardiovascular system while simultaneously increasing behaviors that compound the danger, including smoking and failing to take medicines. Lowering the modifiable risks above is, unsurprisingly, one of the best ways to fight cardiovascular disease. Managing cholesterol, blood pressure, and diabetes can help. Cutting smoking and lowering alcohol intake can make a big difference. Getting help with mental health (and getting a good night’s sleep) may help your heart relax as well. Maintaining a healthy weight through a good diet and dynamic exercise is vital. Unfortunately, without management, cardiovascular disease is more like a desert than a dessert: it can kill you. Staff Writer / Editor Benton Lowey-Ball, BS, BFA
References: Centers for Disease Control and Prevention. (July 19, 2021). Coronary artery disease (CAD). U.S. Department of Health and Human Services. https://www.cdc.gov/heartdisease/coronary_ad.htm National Center for Chronic Disease Prevention and Health Promotion, Division for Heart Disease and Stroke Prevention. (May 15, 2023). About heart disease. U.S. Department of Health and Human Services. https://www.cdc.gov/heartdisease/about.htm American Heart Association. (May 31, 2017). What is cardiovascular disease? https://www.heart.org/en/health-topics/consumer-healthcare/what-is-cardiovascular-disease Tsao, C. W., Aday, A. W., Almarzooq, Z. I., Alonso, A., Beaton, A. Z., Bittencourt, M. S., … & American Heart Association Council on Epidemiology and Prevention Statistics Committee and Stroke Statistics Subcommittee. (2022). Heart disease and stroke statistics—2022 update: a report from the American Heart Association. Circulation, 145(8), e153-e639. https://www.ahajournals.org/doi/full/10.1161/CIR.0000000000001123 National Heart, Lung, and Blood Institute. (n.d). Heart and vascular diseases. U.S. Department of Health and Human Services. https://www.nhlbi.nih.gov/science/heart-and-vascular-diseases Accessed on September 12, 2023. The World Health Organization. (June 11, 2021). Cardiovascular diseases (CVD). https://www.who.int/news-room/fact-sheets/detail/cardiovascular-diseases-(cvds)
Scroll down to listen to this article.
Listen to the article here:
What do Star Wars, Nazi-occupied France, and surge protectors have in common? We root for the resistance to win! But what if the resistance is evil and bad? Meet resistant hypertension. This little devil is a special, particularly damning form of hypertension that resists medications. Not just one or two medications, either! Resistant hypertension avoids at least three separate medications of three separate types (called classes)! Resistant hypertension is when blood pressure remains over 140/90 mmHg while seated, even when the patient is taking the maximum tolerated dose of three or more different classes of hypertension medications. It can damage the heart, eyes, and kidneys and lead to heart attack, stroke, end-stage renal disease, and death. It can be caused by a narrowing of the veins, but the prevalence isn’t narrow at all. It affects 6-9 million Americans, with the highest incidence in Black males. A few conditions are associated with resistant hypertension, including diabetes, obesity, and chronic kidney disease. To understand how this disease works, we must first understand how blood pressure works. Blood pressure is controlled by three main components: heart rate, volume pumped, and blood vessel size. This may seem like a simple system, but each of these three components are affected by a myriad of body systems. Think of it like trying to maintain peace in the middle east. It might seem like you could balance the needs of religion, economics, tradition, and foreign influence, but it turns out: no. Other big actors in the blood pressure realm include the brain and kidneys. The brain directs other organs how to act and the kidneys regulate the fluid in the bloodstream (which we call blood). On top of these big organs, blood pressure is affected by interconnected systems, genes, inflammation, salt, even the bacteria in our gut! One of the biggest systems involved with blood pressure is the Renin-Angiotensin-Aldosterone System, or RAAS (or RAS). This system involves the kidneys and uses hormones to regulate blood pressure. It relies on a few key hormones and enzymes, and is also affected by other systems like the natriuretic peptide system and the brain. In hypertension, one or more of these systems no longer functions properly. We have four major classes of medication to help get the body back on track. Long-acting calcium channel blockers (CCB) reduce the amount that the heart and arteries can contract, relaxing the system. Angiotensin is a hormone that causes blood vessels to narrow. Angiotensin-converting enzyme inhibitors (ACEI) block angiotensin from being made and angiotensin receptor blockers (ARB) block it from acting on blood vessels. Finally, diuretic medications remove water and salt from the blood, lowering the volume of fluid that the heart pumps. Each of these medications targets the body in slightly different ways. Different medications work better for some people, and side effects may present differently. A good doctor will look for a blood pressure medication (or two (or three (or more))) that brings blood pressure to healthy levels without too many side effects. When we do not achieve healthy blood pressure levels even at the maximum tolerated dose of three or more medications we have resistant hypertension. Patients with resistant hypertension are at a higher risk of major cardiac events because they can’t get blood pressure under control with available medications. Prolonged high blood pressure leads to damage throughout the cardiovascular system. So what can be done? The best first step is to lower modifiable risks. This is actually a good first step for literally anything that is dangerous. Weight loss is a good opening move if you are obese. Lowering alcohol and salt intake may help. Talking to a doctor about any medications or conditions that may be raising blood pressure is important. Finally, clinical trials may be underway to look for specialty medications that target those with resistant hypertension. Hopefully we can find a way to crush resistance without succumbing to the dark side of the force (or becoming nazis). Staff Writer / Editor Benton Lowey-Ball, BS, BFA
References: Harrison, D. G., Coffman, T. M., & Wilcox, C. S. (2021). Pathophysiology of hypertension: the mosaic theory and beyond. Circulation research, 128(7), 847-863. https://doi.org/10.1161/CIRCRESAHA.121.318082 Myat, A., Redwood, S. R., Qureshi, A. C., Spertus, J. A., & Williams, B. (2012). Resistant hypertension. Bmj, 345. https://doi.org/10.1136/bmj.e7473 Sarafidis, P. A., Georgianos, P., & Bakris, G. L. (2013). Resistant hypertension—its identification and epidemiology. Nature Reviews Nephrology, 9(1), 51-58. https://www.nature.com/articles/nrneph.2012.260
Listen to the article here:
Sometimes when I’m desperately trying to fall asleep I instead think of all the things that might kill me. Alligators, drunk drivers, hurricanes, and running out of cookies usually top the list. Do you know what doesn’t top the list? High blood pressure. It really should though. High blood pressure is a leading preventable cause of premature death, affecting well over a billion people worldwide and causing upwards of 9 million deaths a year. Maybe the alligators can chew on those facts for a while. So what is high blood pressure, why is it such a big deal, why do we get it, and what can we do? High blood pressure is exactly what it sounds like; when the blood in your arteries is being forced through more strongly than normal. The medical name for high blood pressure is hypertension. Hyper– means over or above, and -tension, in this case, indicates the stress of your arteries. Hypertension is excessive stress on your arteries. Blood pressure can be split into two numbers, systolic and diastolic. These refer to the action of the heart, where systolic is the contracted, pumping blood pressure, and diastolic is the relaxed blood pressure. When you get your blood pressure checked, these are reported as two numbers “over” each other. A reading of 140/90 mmHg or higher is high blood pressure, but there is an increased risk of complications with blood pressure above 120/80 mmHg. High blood pressure is particularly dangerous. It is easy to see why: the bloodstream is how we deliver oxygen to the cells, and it touches every cell in the entire body. Two of the biggest dangers with elevated blood pressure are ischemic heart disease and stroke, conditions where the blood supply doesn’t reach the heart or brain. High blood pressure can also cause brain bleeds, chronic kidney damage, and other types of heart damage. All of these organs are vital to our survival, so a condition that potentially damages all of them is life-threatening. What are the causes of high blood pressure? High blood pressure is calculated the same as in any pipe at its most basic level. The amount of blood coming out of the heart is counteracted by the resistance from the arteries. More output or more resistance makes blood pressure rise. High blood pressure on its own isn’t bad, it’s adaptive for critical situations. When we see a lion and it charges us, we become stressed and initiate the sympathetic nervous system, also known as fight, flight, and freeze. Part of this system’s job is to constrict blood vessels and raise the heart rate to deliver large amounts of oxygen to cells. We see damage when we have high blood pressure for long amounts of time. Some body systems that cause prolonged elevations in blood pressure are: These are the major players in primary or essential hypertension. Secondary hypertension is caused by another identifiable disease, like kidney disease. So what can we do? Some outcomes depend on things we can’t easily change, like access to quality healthcare and blood pressure medication. Many lifestyle options can be changed to improve our blood pressure: Even though we have good evidence for lifestyle changes lowering blood pressure, the biggest difference between countries in terms of controlling blood pressure is access to medicine. Blood pressure medicines have saved countless lives and helped stem the blood tide of hypertension. There are several types of blood pressure medicines on the market. Diuretics get rid of sodium and water in the blood. Angiotensin-converting-enzyme (ACE) inhibitors and Angiotensin-receptor blockers (ARB) help ease inflammation, relax the blood vessels, and keep them from constricting. Calcium channel blockers reduce heart rate. These all have side effects, but the biggest challenge with them is that they are daily oral medications, which can be forgotten, missed, or hard to adhere to. Longer-term solutions are in clinical trials and may be available to you if you qualify. So don’t sleep on your high blood pressure. Check with your local ENCORE Research office to see what studies are enrolling. See ya’ later, alligators! Staff Writer / Editor Benton Lowey-Ball, BS, BFA
Sources: Harrison, D. G., Coffman, T. M., & Wilcox, C. S. (2021). Pathophysiology of hypertension: the mosaic theory and beyond. Circulation research, 128(7), 847-863. https://www.ahajournals.org/doi/full/10.1161/CIRCRESAHA.121.318082 Lifton, R. P., Gharavi, A. G., & Geller, D. S. (2001). Molecular mechanisms of human hypertension. Cell, 104(4), 545-556. https://doi.org/10.1016/S0092-8674(01)00241-0 Mills, K. T., Stefanescu, A., & He, J. (2020). The global epidemiology of hypertension. Nature Reviews Nephrology, 16(4), 223-237. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7998524/
Listen to the article here:
Hypertension is one of the most prevalent conditions on the planet. Scientists estimate that it affects 30-45% of adults, somewhere over a billion people! Hypertension is the chronic elevation of blood pressure. The CDC defines it as above 130 mmHg systolic or above 80 mmHg diastolic. For short periods of time, elevated blood pressure can be useful – for exercise, say. People can have high blood pressure for years without symptoms. For long periods of time, however, hypertension is deadly serious. Unfortunately, living with high blood pressure can lead to a host of problems. Hypertension can lead to heart attack and stroke, and damage to the heart, brain, kidneys, and even eyes! Everyone is at risk of high blood pressure. In America, men have a higher likelihood of hypertension. There are also differences in ethnicity and race, non-Hispanic Black or African American adults are at the highest risk. Unfortunately, even the lowest risk categories still have around a 40% prevalence of high blood pressure. Clearly this is a large issue in America and around the world. The big culprit behind hypertension is the Renin–angiotensin–aldosterone system (RAAS). RAAS is a critical system for maintaining blood pressure. It regulates two primary factors: the amount of blood and how constricted blood vessels are. It does this through the kidney, liver, and adrenal gland (just above the kidneys). In response to body signals, the kidneys release an enzyme to the liver. In response, the liver produces the hormone angiotensin I. Another enzyme, angiotensin-converting enzyme (ACE) converts this to angiotensin II, which goes to work. Angiotensin II has wide-ranging effects to increase sodium and water retention. It also causes blood vessels to constrict. Angiotensin II is very short-lived, only lasting 1-2 minutes. One of its many effects is to get the adrenal gland to produce aldosterone. Aldosterone has similar effects as angiotensin II, but instead of a few minutes, it takes hours or days to take effect. The end result is that two major hormones – one fast-acting and one slow-acting – cause high blood pressure. There are many medications available to fight hypertension. Most of these, such as diuretics or beta-blockers, have wide-ranging side effects. This is because they are system-wide, indiscriminate actors on the body. Beta-blockers, for instance, slow the heart. This is helpful in lowering blood pressure but obviously leads to other effects on the body. RAAS-acting specific medications may be more helpful in combating hypertension with minimal side effects. ACE inhibitors, for instance, stop the fast-acting angiotensin II from having its effect on the body. This targeted approach to hypertension can lead to fewer side effects in some patients. Unfortunately, by acting on only the fast-acting portion of RAAS, they must be taken daily. Even worse, a few missed doses can have longer-term effects on blood pressure. Luckily, researchers are investigating other targeted methods of reducing the effect of RAAS, and blood pressure! Keep an eye out for a clinical research study to help investigate this exciting part of the fight against hypertension. Written by: Benton Lowey-Ball, B.S. Behavioral Neuroscience
Sources Fountain, J. H., & Lappin, S. L. (2017). Physiology, renin angiotensin system. National Center for Chronic Disease Prevention and Health Promotion, Division for Heart Disease and Stroke Prevention. (September 27, 2027). Facts about hypertension. U.S. Department of Health and Human Services. https://www.cdc.gov/bloodpressure/facts.htm
Listen to the article here: