GRID VIEW
The eyes are the windows to the soul. But what happens when those windows don’t get properly cleaned? They might get scratchy, stingy, blurry, and discolored. Dry eye disease is when tears don’t adequately lubricate the eye. Symptoms include scratchy burning or stinging in the eyes, red eyes, sensitivity to light, and blurry vision. This disease affects 5%-30% of the world population and is more common in women and those above 50 years old. Dry eye is a multifactorial disease, meaning multiple things may have a hand in causing it. To understand what might be going wrong, we first have to understand a little about how the eye works.
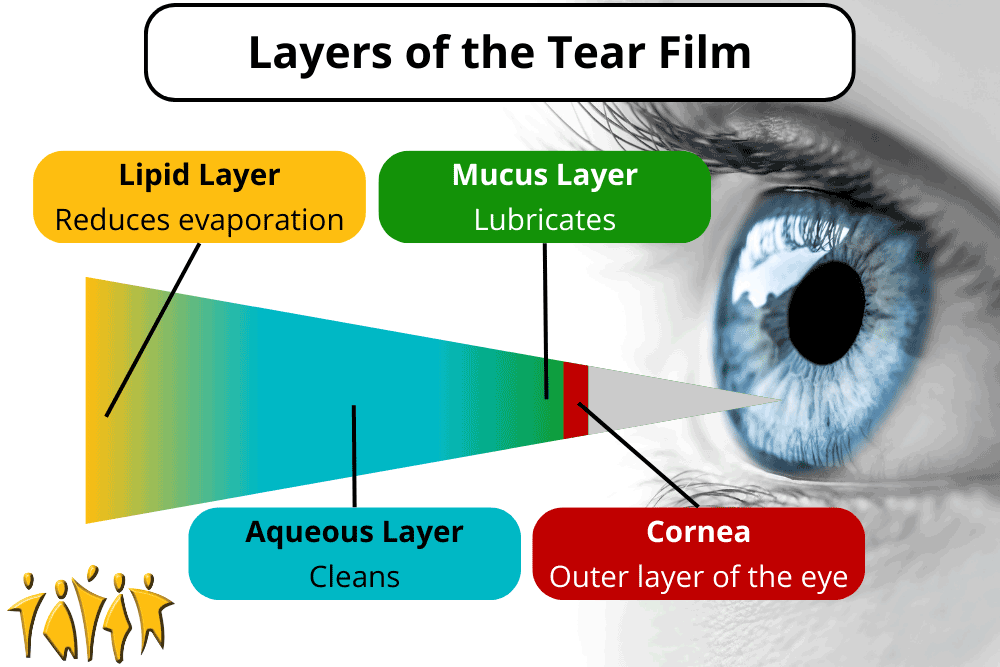
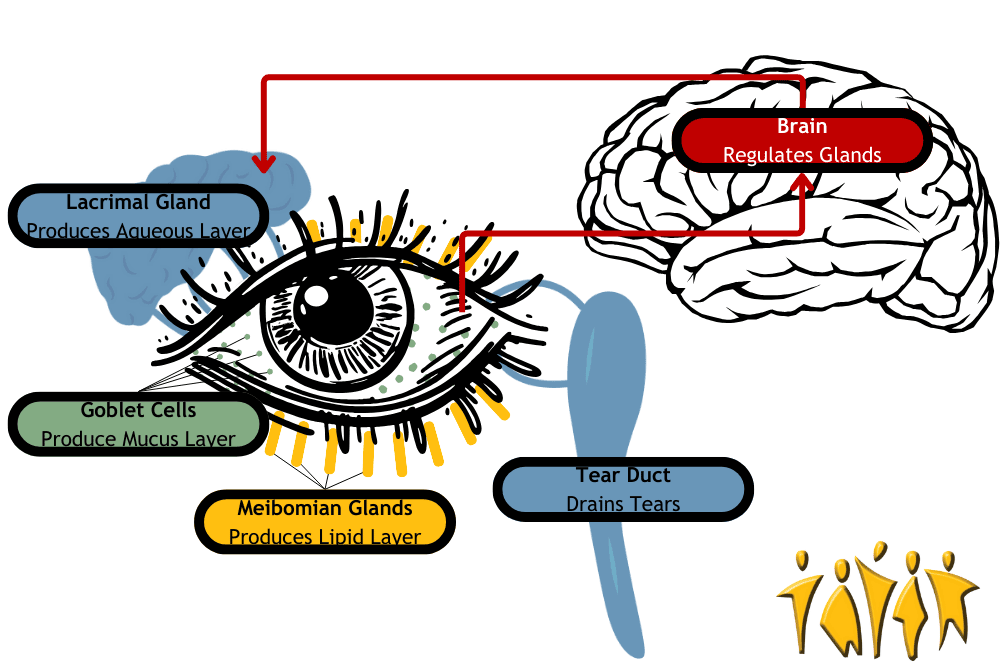
The eye is lubricated by a 3-layered film called the tear film on the outside. That’s tear like near, not tear like hair. The layers, from inner to outer, are the mucus layer, aqueous (water) layer, and lipid (oil) layer. These aren’t hard, distinct layers, but each has a separate purpose. The mucus layer is secreted by goblet cells located on the surface of the eye and lubricates it. The aqueous (water) layer is secreted by the lacrimal gland and keeps everything clean. It is susceptible to evaporation, which is where the lipid (oil) layer plays a part. The lipid layer is oily, which resists evaporation and is secreted by meibomian glands on the edge of the eyeball. Together, these layers act like a crew of window washers to keep the eye lubricated and clean. Don’t let all the vocabulary make you googly-eyed: the lacrimal gland, goblet cells, and meibomian glands just produce different types of eye fluids. They work together to produce the tear film, but they don’t work alone. The brain receives moisture signals from the eye and sends signals to the glands to keep the eye moist. The eyelids spread the tear film and help prevent evaporation. Finally, the surface of the eye itself needs to be clean and healthy. Together, these components make up the lacrimal functional unit. Disruptions to this system are the cause of dry eye disorder. Problems can be divided into broad categories, but each can overlap and lead to problems with other parts of the lacrimal functional unit.
Problems can originate in the nerves to and from the brain. These can become inflamed or attacked by immune cells such as with Sjogren’s syndrome. When the nerves from the brain to the lacrimal gland are disturbed, tear production might be reduced. When the sensory nerves from the eye to the brain are disrupted, the brain doesn’t know to tell the lacrimal glands to secrete tears and keep the tear film intact. Nerve response can also be disrupted permanently by long-term contact lens use and temporarily by laser surgery. The cells of the eye itself can also be damaged. Epithelial (surface) cells need to interface smoothly with the tear film. The aqueous (water) layer can be deficient – you may not produce enough tears. This can be due to inflammation and autoimmune problems (as above), obstructed glands, nerve damage, and more. Medicines like antihistamines, beta-blockers, and diuretics can also reduce the aqueous layer. Allergies can cause dry eye, so the fact that antihistamines can cause it too is deeply eye-ronic. Finally, tears may evaporate too quickly. This is called tear instability or evaporative dry eye and is usually due to a problem with the oil layer. Other evaporative problems include eyelid problems, gland dysfunction, decreased blinking, vitamin A / omega-3 deficiency, and environmental problems (like wind and smoke). To help with dry eye we can look at three methods: environmental, surgical, and medical. Environmental relief can be found by avoiding dry, dusty, and smoky air while ensuring you get enough vitamin A and Omega-3. Surgical blocking of the drainage tear duct can keep moisture on the eye surface longer. Medical solutions include different types of eye drops. Some mimic tears, and some deliver medicine. For severe and chronic problems, there are two major medications: cyclosporine and nerve growth factor (NGF). Cyclosporine is an immunosuppressive drug that can relieve inflammation in the nerves and glands. Nerve growth factor is an amazing medical category that can regenerate damaged nerve fibers and can heal surface epithelial cells. With new clinical trials on the horizon, we can peer through the window to new relief for dry eyes! Staff Writer / Editor Benton Lowey-Ball, BS, BFA
References: Lemp, M. A., & Foulks, G. N. (2007). The definition and classification of dry eye disease. Ocul Surf, 5(2), 75-92. Mantelli, F., Massaro‐Giordano, M., Macchi, I., Lambiase, A., & Bonini, S. (2013). The cellular mechanisms of dry eye: from pathogenesis to treatment. Journal of cellular physiology, 228(12), 2253-2256. https://onlinelibrary.wiley.com/doi/pdf/10.1002/jcp.24398 National Eye Institute. (April 8, 2022). Dry Eye. National Institute of Health https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/dry-eye
Scroll down to listen to this article.
Listen to the article here:
Vision is our main way of interacting with the world, and it can be debilitating when our vision deteriorates. Unfortunately, presbyopia – the gradual loss of ability to focus on nearby objects – is basically inevitable. Presbyopia affects nearly 25% of the world population; almost 2 billion people. People usually see symptoms in their 40s, but the path starts in childhood. The exact cause of presbyopia is unknown, but the effects are well documented. The eye’s lens is the bit that changes shape, allowing us to focus at different distances. During childhood, the lens gradually becomes less flexible. Since it can’t change shape as easily, we stop being able to focus as rapidly and accurately. It gets more difficult to focus at close or mid-lengths. There are four broad methods suggested for increasing focal range, each with its own trade-off. Changing focus over time is the first method. Think of it like having several pairs of glasses. When focusing on close things you might use readers. Different glasses may be used for mid-length, or distance viewing. This is what our eyes do naturally (when we’re young at least!). So far there are no pharmaceutical or implantable devices that can accomplish this. Using several glasses is a good – if bulky – approximation for millions of people, however. Changing focus depending on where you look is the second method. Bifocals are the classic example. This solution is quick and convenient. There are downsides, however. Changing from near to mid-focus can be jarring, vision can be blurry, and eye strain occurs sometimes. One often overlooked issue is that bifocals can introduce other dangers, such as falls due to unfocused areas near the feet when walking. Changing focus between eyes is an interesting method. With this approach, one eye is corrected for close vision, and the other stays focused at a distance. Each eye only focuses narrowly, but together you can see across a wide range. Even though this is easy to try by putting in only one contact lens, it can be hard to get used to and lead to a loss of binocular vision. Judging distances of objects may be more difficult with this method, and it can be uncomfortable for some people. The final method is to increase the focal range across distances. This is an innovative method where the eyes are changed to have more in-focus at the same time. If you’ve ever had an eye exam where they dilate your pupils, this is the opposite. The pupils are artificially constricted. This extends your depth of field, making it easier to focus on things near and far at the same time! Some side effects may include a loss in quality and contrast, and a loss of low-light sensitivity. One of the big hurdles researchers have is the precision required to pull this off successfully. Methods to induce increasing focal range can be permanent, such as with implanted lenses; but mitigation of side effects may be easiest with special eye drops. Some of these eye drops are being tested currently in clinical trials. With so many different angles to attack presbyopia, and volunteers helping with clinical trials, we may be looking at a universal treatment soon! Written by: Benton Lowey-Ball, B.S. Behavioral Neuroscience
Source: Chang, D. H., & Waring, G. O. (2021). Presbyopia Treatments by Mechanism of Action: A New Classification System Based on a Review of the Literature. Clinical Ophthalmology (Auckland, NZ), 15, 3733.
The eye is a fragile and carefully balanced organ. At the very front of the eye is a fluid-filled chamber called the anterior chamber. This is located between the clear cornea at the front and the pupil, where light enters the rest of the eye. The fluid that fills this area is called the aqueous humor. The aqueous humor is critically important for cleaning and bringing nutrients to the lens. It is like a clear version of blood. Another key job the aqueous humor performs is maintaining eye pressure. The pressure in the eye needs to be maintained within a very specific range (12-22 mm Hg). Aqueous humor continuously flows through the front of the eye at a very slow rate (like blood, but slower). When the flow rate out of the eye gets disrupted, eye pressure increases. Doctors call high eye pressure ocular hypertension. The major characteristic is increased eye pressure without other symptoms. When eye pressure causes damage to the optic nerve, we call it glaucoma. Glaucoma can occur in two ways, closed angle or open angle. Closed angle is sudden and a medical emergency. Open angle makes up almost all cases of glaucoma and is gradual in onset. Typical symptoms of open angle glaucoma are vision problems in the middle of sight. These can include trouble with reading, seeing faces, walking, and driving. Both types will cause permanent blindness if untreated. Open angle glaucoma can happen to anyone, but is much more common with adults over 60 years old. Most cases are females, and black and Asian populations experience higher rates of the condition. There are several underlying reasons for open-angle glaucoma: vascular, anatomical, genetic, or immune. Because of this wide spread of causes, there are several risk factors: Several treatments are available for glaucoma. These include surgical and medication-based treatments, and surgically implanted medications. The goal of all treatments is to increase the flow of fluid out, decrease the amount of fluid coming in, or to decrease the volume of the anterior chamber. Medications are quite effective when taken properly. Unfortunately, fewer than one third of patients adhere to doctor recommendations for glaucoma eye drops after a year. This is in spite of the condition being progressive in nature and leading to blindness. Effective implanted medication delivery systems may provide better outcomes for patients. To get involved in the latest glaucoma research, contact our Nature Coast Crystal River office.
Sources: Allison, K., Patel, D., & Alabi, O. (2020). Epidemiology of glaucoma: the past, present, and predictions for the future. Cureus, 12(11). Li, F., Huang, W., & Zhang, X. (2018). Efficacy and safety of different regimens for primary open‐angle glaucoma or ocular hypertension: A systematic review and network meta‐analysis. Acta ophthalmologica, 96(3), e277-e284. Robin, A. L., & Muir, K. W. (2019). Medication adherence in patients with ocular hypertension or glaucoma. Expert Review of Ophthalmology, 14(4-5), 199-210.
Listen to the article here:
Glaucoma is a common eye disease that can gradually steal your vision. The term glaucoma refers to a collection of eye diseases that damage the optic nerve. This damage can lead to permanent vision loss or even total blindness. Glaucoma is considered a major cause of blindness in the general population.
A major concern is that glaucoma often presents no early symptoms but continues to cause gradual, un-reversable damage. In most cases, glaucoma is diagnosed in people who are older than 40 but can still develop at an earlier age. An estimated 3.54% of adults between 40 and 80 years have been diagnosed with some type of glaucoma.
Causes Of Glaucoma
In most types of glaucoma, the eye’s drainage system becomes clogged so the intraocular fluid cannot drain. As the fluid builds up, it causes pressure to build inside the eye. High pressure damages the sensitive optic nerve and results in vision loss.
People are more likely to develop glaucoma if they:
- Are over the age of 40
- Have a family history of glaucoma
- Have high blood pressure, heart disease, diabetes, or sickle cell anemia
- Are of African American, Irish, Russian, Japanese, Hispanic, Inuit, or Scandinavian descent
- Take certain steroid medications such as prednisone
- Have had an injury to your eye or eyes
- Have high eye pressure (ocular hypertension)
Current Treatments Available
Unfortunately, there is not currently a cure for glaucoma. However, there are several therapies that can help reduce eye pressure and the rate of damage to the optic nerve. Current approved treatment options for glaucoma include eyedrops, oral medications, laser surgery, or microsurgery.
Clinical Research Advancements
New clinical trials for glaucoma are focused on more innovative ways to treat the disease. Researchers are studying everything from electric current stimulation to slow release eye implants to help find relief for patients with glaucoma.
You can help advance medical research by participating in a clinical trial! Contact any of our offices to see what clinical trials are enrolling today.
References:
https://www.aaojournal.org/article/S0161-6420(14)00433-3/abstract
https://www.mayoclinic.org/diseases-conditions/glaucoma/symptoms-causes/syc-20372839
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4927811/





