A colonoscopy is used to detect any changes in the large intestine and rectum. A long flexible tube, called a colonoscope, is inserted into the rectum during the exam. At the end of the tube is a tiny video camera that allows the provider to view the inside of the colon. During the colonoscopy, your provider may also remove some abnormal tissue or take tissue samples if needed. It is common practice to receive a sedative before the exam to make you feel more comfortable, relaxed and decrease the chance of any pain. Both men and women need colonoscopies around the age of 50. If you are at a high risk for developing colorectal cancer, cancer that affects the colon and the rectum, your provider may ask you to receive a colonoscopy at an earlier age. You should reach out to your healthcare provider if you are having any symptoms of colorectal cancer because getting a colonoscopy could help prevent serious illness or even death. Symptoms include: There are many reasons why a colonoscopy is important. The main reason, as mentioned previously, is to test for colon cancer. Secondly, a colonoscopy investigates any problems with your intestines. If you are experiencing any abdominal pain or intestinal problems, let your doctor know beforehand. This way, your doctor can assess and find the answers to why you may be experiencing these issues. A colonoscopy also looks for abnormal tissues called polyps. A follow up colonoscopy might be necessary to remove all polyps to reduce your risk of colon cancer. Colon cancer is the third most common cancer among men and women over the age of 50. More clinical trials are needed in order to reduce this number and save lives. If you are in need of a colonoscopy, you may qualify for an enrolling study at one of our ENCORE Research Group locations. Participating in research trials have many benefits, including free medical attention, access to new technology and the chance to move medicine forward creating a healthier nation. Source: Borland Groover, American Cancer Society
What is a Colonoscopy?
Who Needs One and When?
Why are They Important?
Are there any Enrolling Studies at ENCORE Research Group?
GRID VIEW
The questions that have many people puzzled are finally going to be answered: What is gluten and is it actually bad for you? Gluten is a mixture of two types of proteins. It is responsible for the elastic texture of dough. These proteins are commonly found in wheat, rye, oats and barley. Gluten helps food keep its shape and acts like a glue that holds certain foods together. For those with celiac disease, gluten can be particularly dangerous. Gluten triggers an immune response in people with the disease, resulting in damages in the lining of the small intestine. These damages can obstruct a person’s ability to absorb nutrients from food and lead to problems like osteoporosis, infertility, nerve damage, and seizures. Adults with celiac disease show many digestive and other symptoms including: Digestive symptoms: Non-Digestive Symptoms: Gluten can be found in many different kinds of foods. It may be present in more foods than you think. The main foods to look out for which contain high amounts of gluten are processed foods, such as canned or boxed items, sweets, including cakes, pies and candies, cereals, bread, beer, pasta and more. Currently, the only treatment for celiac disease is to completely eradicate gluten from a person’s diet, which can be difficult. In order to help those suffering from this disease, it is imperative to do more research including participating in clinical trials. If you have celiac disease and want to be at the forefront of medicine, click the “enrolling studies” tab for more information about current clinical trials. Source: Harvard Health, Celiac Disease Foundation
What is H. pylori? H. pylori is short for helicobacter pylori, and it is a type of bacteria that grows in the stomach and can cause infection. This infection might be a lot more common than you think. With approximately 30-40% of the United States’ population containing the bacteria, there is no question as to how important more research needs to be done to combat it. If left untreated, H. pylori may cause peptic ulcers, gastritis, or stomach cancer. However, it often does not have any symptoms at all. What are the signs and symptoms? Many who contract H. pylori experience no symptoms at all, however when symptoms do occur, here is what you can expect: How do I get H. Pylori? Contracting H. pylori is common, and even more prevalent in developing countries. Some factors may increase your risk of infection like sharing a small, crowded living space, no access to clean water, and living with someone who has H. pylori. Some ways to reduce your risk of infection are to wash your hands before eating and after using the bathroom. Eat food that has been properly prepared and drink clean water. When should I see a doctor? As a good rule of thumb, you should always see a doctor if you have worsening stomach pains. You should also see a doctor if you have: Researchers are studying new ways to treat H. pylori infection and ENCORE Research Group is conducting some of these clinical trials. If you would like to help move research and medicine forward, visit our enrolling studies page to see clinical trials that are enrolling now in your area. Source: U.S. National Library on Medicine, Everyday Health, American Journal of Gastroenterology
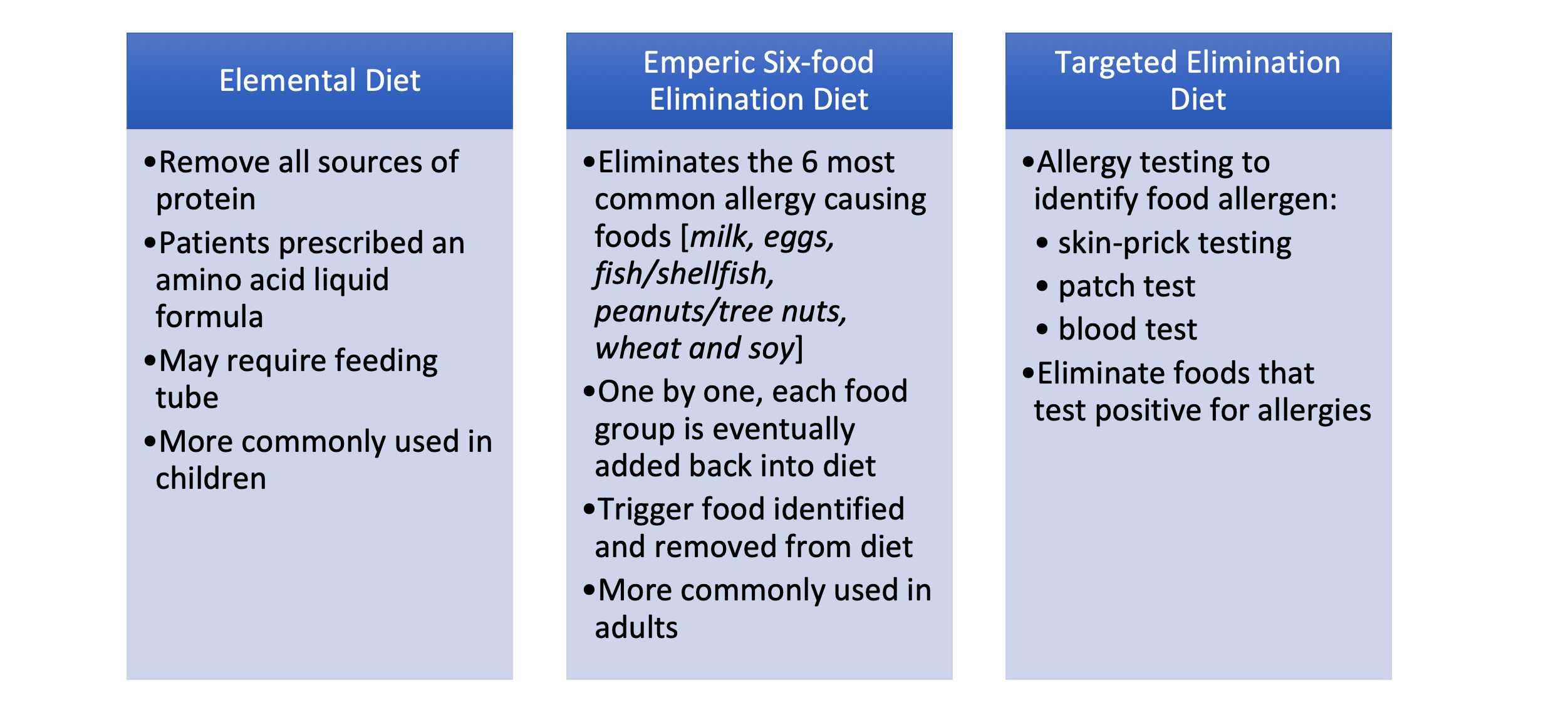
Eosinophilic Esophagitis (EoE) is a chronic, immune-mediated disorder. It occurs in approximately 1 in 10,000 people and affects people of all age groups, with males being affected more frequently. EOE is associated with food allergies or other allergens, causing eosinophils (type of white blood cell) to migrate from the bone marrow (via blood) and settle in the esophagus causing inflammation to the esophagus. No one knows exactly why EoE occurs. People with EoE tend to have allergic conditions such asthma, seasonal allergies, allergic rhinitis, and eczema. Symptoms of EoE: EoE symptoms can overlap with symptoms of a condition called gastroesophageal reflux disease (GERD). Patients with EoE experience symptoms described as, If EoE is not controlled, the eosinophils will cause damage to the esophagus. Sometimes food that gets stuck in the esophagus (food impaction) may require emergency removal. How is EoE Diagnosed? If you have symptoms of EoE, your doctor will order a procedure called an endoscopy (EGD). An EGD is required to confirm the diagnosis and is performed by a specialist called a gastroenterologist. Patients are sedated for this procedure and a small flexible tube with a light and camera on the tip is inserted into the patient’s mouth. During the endoscopy, several biopsies of the esophagus will be taken and sent to the laboratory for analysis under a high-power microscope. EoE is confirmed when 15 or more eosinophils per high-power field are found (≥15 Eos/hpf). How is EoE Treated? Many patients with EoE are initially treated for GERD using a medication called a proton pump inhibitor (PPI). However, most EoE patients do no respond to anti-GERD treatment. Treatment with PPIs is given for a minimum of 8 weeks followed by a repeat EGD and biopsy. If the eosinophil count remains elevated (≥15/hpf), the diagnosis of EoE is confirmed and a different treatment is given. Patients with EoE are often referred to an allergy specialist for evaluation. Allergy testing can be done to identify which foods are triggering the EoE. Treatment for EoE usually includes dietary management and/or medication, or treatment on a clinical trial. If you have symptoms of EoE, it is important that you seek medical care and discuss your symptoms with your doctor. You can also learn more about EoE from advocacy organizations such as Apfed (apfed.org), or by joining an on-line patient communities such as Healtheo360 (healtheo360.com). Research is currently being conducted around the United States for this condition. Here at ENCORE Research Group we have 3 research sites with a new opportunity for people who have Eosinophilic Esophagitis. If you’re interested in learning more about this research, please contact your local research office below! Jacksonville: ENCORE Borland Groover Clinical Research 904-680-0872 Fleming Island Fleming Island Center for Clinical Research 904-621-0390 Inverness: Nature Coast Clinical Research 352-341-2100

At some point in our lives we have all experienced acid reflux. Maybe it was after eating something spicy, or any acidic food like a tomato or certain dairy products and you felt a burning sensation in your throat. GERD, or gastroesophageal reflux disease is similar to acid reflux. GERD is a long-term condition where acid from your stomach overflows into the esophagus. If you experience acid reflux that occurs more than twice a week, your doctor may diagnose you with GERD. If you are experiencing these below symptoms more than twice a week, it may be time to see a doctor. Although GERD is a common condition affecting over 3 million Americans per year, if left untreated, it can lead to serious medical conditions. With certain lifestyle changes and medication, GERD can be treated. However, more research is needed to understand why there is a steady increase in Americans with GERD. Currently, ENCORE Research Group has enrolling studies for GERD taking place in Crystal River and Jacksonville. Visit our Enrolling Studies page to see what’s enrolling at a research site near you. Source: Medical News Today, Medline Plus
Ulcerative Colitis is a rare inflammatory bowel disease (IBD) with less than 200,000 cases per year. Ulcerative colitis can cause long-term effects on the body including inflammation and ulcers in the digestive tract. This can affect the innermost lining of the large intestine as well as the rectum. The symptoms of ulcerative colitis can range from mild to severe. Symptoms include rectal bleeding, bloody diarrhea, abdominal cramps and pain. Those who have Ulcerative Colitis are also at a greater risk of developing colon cancer. Doctors usually diagnose the different types of ulcerative colitis according to its location in the large intestine. The different types of ulcerative colitis include: Ulcerative Proctitis This is when the inflammation is in the area closest to the rectum. Rectal bleeding may be a sign of this disease, and it tends to be the mildest form. Proctosigmoiditis This type of ulcerative colitis is confined to the rectum as well as the lower end of the colon (sigmoid colon). Symptoms include abdominal cramps, bloody diarrhea, and the inability to move bowels, even though you feel as though you need to. Left-sided colitis If you have sharp pain on your left side, bloody diarrhea, abdominal cramping or weight loss, you may be experiencing left-sided colitis. This happens when inflammation extends from the rectum through the sigmoid and descending colon. Pancolitis Pancolitis often affects the entire colon. This can cause severe bloody diarrhea, abdominal cramps and pain, fatigue and weight loss. Acute severe ulcerative colitis This form of colitis is rare. It is a severe form and it affects the entire colon. It can cause severe pain, profuse bloody diarrhea, fever and complete loss of appetite. Although rare, ulcerative colitis can cause an abundance of health problems. It is imperative to participate in clinical trials in order to move medicine forward and help find effective treatments for ulcerative colitis sufferers. Resources: Cleveland Clinic, Crohn’s and Colitis
Crohn’s disease is a chronic irritable bowel disease (IBD). In those with crohn’s disease, an abnormal immune system causes chronic inflammation in the digestive tract. IBD affects nearly 3 million Americans, and there is still no known cure.
Symptoms of Crohn’s Disease
A person living with crohn’s disease can experience many symptoms and the severity can range from no pain at all to immobilizing. The symptoms include:
- Diarrhea
- Abdominal pain
- Cramping
- Weight Loss
- Blood in Stools
- Fatigue
- Nausea and vomiting
- No appetite
- Anemia
- Fever
Long-Term effects of Crohn’s Disease
Living with crohn’s disease can take its toll on the body long term. If left unmanaged, crohn’s disease can worsen and cause extreme pain and health concerns. Over time, crohn’s disease can cause severe damage to the GI tract. This can lead to:
- Fistulas. When excessive inflammation causes ulcers to form on the intestine, a fistula can form. A fistula is when two parts of the intestine connect to form a tunnel to drain the pus from the infected area.
- Intestinal Abscesses. This is caused by an excess of bacteria in the abdomen.
- Intestinal Blockages. This is a blockage that keeps food or liquid from passing through the small or large intestine. Symptoms can include severe abdominal pain, vomiting and inability to pass gas or stool.
- Internal Bleeding. This internal bleeding is caused by tears in the bowel wall due to inflammation in the colon. It is often the cause for diarrhea or bloody stool, a common symptom of crohn’s disease.
Crohn’s disease can be managed and those with the disease can live a very fulfilling life. The main goal of management is to treat the inflammation, which should reduce the severity of the symptoms and hopefully lead to long-term remission.
As mentioned, there is no known cure for crohn’s disease. The only way to find a cure and help those living with crohn’s disease is to participate in clinical trials to further research and hopefully, find a cure.
Resources: Centers for Disease Control and Prevention, Crohn’s and Colitis Foundation, Bladder and Bowel
Chronic pancreatitis is inflammation of the pancreas that does not heal but worsens over time. When you have chronic pancreatitis, your digestive enzymes begin to digest the pancreas itself. The pancreas is a small gland behind the stomach that secretes digestive juices into the small intestine. Eventually, chronic pancreatitis can damage a person’s digestive system and ability to make pancreatic hormones.
Some common causes of chronic pancreatitis are, but not limited to:
- Alcoholism
- Family history
- Autoimmune diseases
- A blocked pancreatic duct
- A genetic mutation such as mutations of the cystic fibrosis
Chronic pancreatitis, if unmanaged, can lead to:
- Diabetes- Chronic pancreatitis causes damage to the insulin-producing cells resulting in diabetes, a chronic condition where there is an abnormally high level of sugar in the blood.
- Pancreatic Cancer- If you have chronic pancreatitis, you are at an increased risk of developing pancreatic cancer by two to three
- Malnutrition- Chronic pancreatitis can cause your pancreas to produce fewer enzymes that are needed to break down and process nutrients from your Overtime, this may lead to malnutrition and significant weight loss.
Although there are many complications that may arise if you are living with chronic pancreatitis, the disease is treatable if caught in time. For chronic pancreatitis the treatments can be a hospital visit to treat dehydration, pain medication and a lifestyle change to a low-fat diet.
According to the type of pancreatitis that you have, other surgeries may be required.
One of the worst symptoms of pancreatitis is the severe abdominal pain. Currently, the only remedy for this is pain medication. In order to better understand and treat this pain more research needs to be done. The goal is to improve the quality of life and the risk of complications when living with pancreatitis.
Sources: MedlinePlus, Pancreatic Cancer Action, National Institute of Diabetes and Digestive and Kidney Diseases, National Pancreatitis foundation
More than just diarrhea…
Inflammatory Bowel Diseases include Crohn’s Disease and Ulcerative Colitis. These diseases cause inflammation in the digestive tract. Both diseases can have similar symptoms such as diarrhea, urgency, abdominal pain and cramping, fatigue, and rectal bleeding.
What’s the difference between Crohn’s and Ulcerative Colitis?
Crohn’s Disease can cause inflammation anywhere in the digestive tract, from the mouth to the anus. Ulcerative Colitis (UC) affects only the colon (also known as large intestine or large bowel). UC causes ulcers along with the inflammation and puts those affected at a higher risk of developing colon cancer.
What causes Ulcerative Colitis?
Physicians used to believe that stress and diet choices caused ulcerative colitis. Physicians now believe that UC was already present, and can be aggravated by these factors.
Research has shown that the immune system plays a role in developing Ulcerative Colitis.
My own immune system is giving me this disease?
There is no clear cause of UC. Medical science shows that an overactive immune system may be to blame. This can lead to continuous inflammation of the colon, and Ulcerative Colitis.
Many of the medicines currently prescribed to treat UC suppress (decrease the activity of) the immune system.
Is there a cure?
There is currently no medical cure for UC. Medical treatment is available to help manage it. American hospitals experience 500,000 visits per year and 46,000 hospitalizations for Ulcerative Colitis. In severe cases, surgical removal of the colon does cure ulcerative colitis.
The Good News
New medicines are now being studied with ENCORE Research to find a cure for UC. Please call for more information, or to schedule an evaluation to see if this is an option for you.
We look forward to talking with you!
Gastroenterology is the medical specialty concerned with the structure and function of the digestive tract (also called gastrointestinal [GI] tract). Some symptoms that can indicate disease or dysfunction of the GI tract include nausea, vomiting, weight loss, heartburn, regurgitation, abdominal pain, abdominal bloating, rectal bleeding, constipation, and diarrhea. Digestion of food and fluids is a very complex process, so persistent symptoms may require a gastroenterologist’s evaluation to determine the cause. Knowing the cause of symptoms can then lead to proper treatment and control or management.
What’s the Difference between IBS and IBD?
Irritable Bowel Syndrome (IBS)
IBS is a common GI disorder that can considerably reduce the quality of life. It affects as many as 5%-20% of individuals worldwide. It occurs more often in women than in men, and is more commonly diagnosed in patients younger than 50 years of age. Symptoms range from diarrhea to constipation, or a combination of the two. Abdominal pain or discomfort often exist alongside abdominal distension.
Diagnosis of IBS is made after obtaining a medical history, physical exam, and diagnostic testing to learn if any disease process is causing the symptoms. There is evidence to show that IBS can be a result of genetics, environment and social learning, dietary or intestinal microorganisms, low-grade inflammation and/or dysfunction of muscular movements, secretions and sensation.
Many patients with IBS ignore their symptoms, believing they are a normal part of everyday life. The good news is that with proper diagnosis, there are ways to treat or manage the symptoms. Don’t ignore persistent symptoms, there is help available.
Inflammatory Bowel Disease (IBD)
IBD is not the same as IBS, and understanding the difference is important for proper treatment. The symptoms can be the same, but the problem causing the symptoms is very different. Inflammatory bowel disease includes Crohn’s Disease (CD) and Ulcerative Colitis (UC). Crohn’s Disease can cause inflammation through the walls of the GI tract and can affect any part of the GI tract. Ulcerative Colitis commonly includes inflammation of the GI mucosa and is limited to the colon (large intestine). Recent research showed that some factors that can lead to IBD includes genetic susceptibility, environment, intestinal microorganisms, and immune responses. Medications are directed at treating the active inflammation, which can then decrease or control the symptoms.
Conclusion
Since symptoms of many GI disorders can be the same, a thorough medical history, physical exam, and proper diagnostic testing is crucial to obtaining a correct diagnosis and treatment. Open communication with your gastroenterologist and health care providers is essential to appropriate management and treatment. Be sure to tell your doctor about symptoms that concern you and new problems that arise. Do not hesitate to ask questions to ensure your understanding of your diagnosis and any treatment prescribed. Being a partner in your health care can lead to a healthier, happier life!
Written By: Julie Baker, RN
Resource: World Journal of Gastroenterology
Gluten Free. This has become a household term. Everyone has heard of gluten free diets, but not everyone comprehends why this distinction is necessary. For people with celiac disease, gluten can be devastating, and it is essential for food labeling to be correct. Celiac disease is an autoimmune disorder where the ingestion of gluten leads to damage in the small intestine. (1) Even ingesting minuscule quantities of gluten, such as crumbs from a toaster, can trigger intestinal damage. This damage can prevent the body from properly absorbing nutrients. Celiac disease is hereditary and is estimated to affect 1% of people worldwide.
There are more than 200 known symptoms of celiac disease, which can make it a nightmare to diagnose. It is estimated that there are 2.5 million undiagnosed Americans. When you mention celiac, most people think of digestive symptoms however, only around one-third of adults with the disorder experience digestive symptoms like diarrhea. Common symptoms include: fatigue, joint pain, arthritis, fatty liver, depression or anxiety, peripheral neuropathy, migraines, canker sores, and skin rash. If left untreated, Celiac disease can lead to many long-term health complications. Unfortunately, the only way to accurately diagnose celiac disease is to have an endoscopic biopsy. Once a diagnosis is made, the challenge of managing the condition begins.
Currently, the only effective treatment for celiac disease is to follow a strict gluten-free diet. However, the future is not bleak. Researchers from around the world are working to find effective pharmaceutical treatments. COUR Pharmaceuticals is researching a drug which aims to reprogram the body’s immune system to tolerate gluten subsequently reversing the signs and symptoms of Celiac disease.(2) Additionally, the Journal of Biological Chemistry notes that scientists have discovered a protein associated with celiac disease can be inactivated, paving the way for new treatment possibilities.(3)
References:
- https://celiac.org/celiac-disease/understanding-celiac-disease-2/what-is-celiac-disease/
- https://www.courpharma.com/pipeline-and-programs/
- https://www.sciencedaily.com/releases/2018/02/180223122343.htm
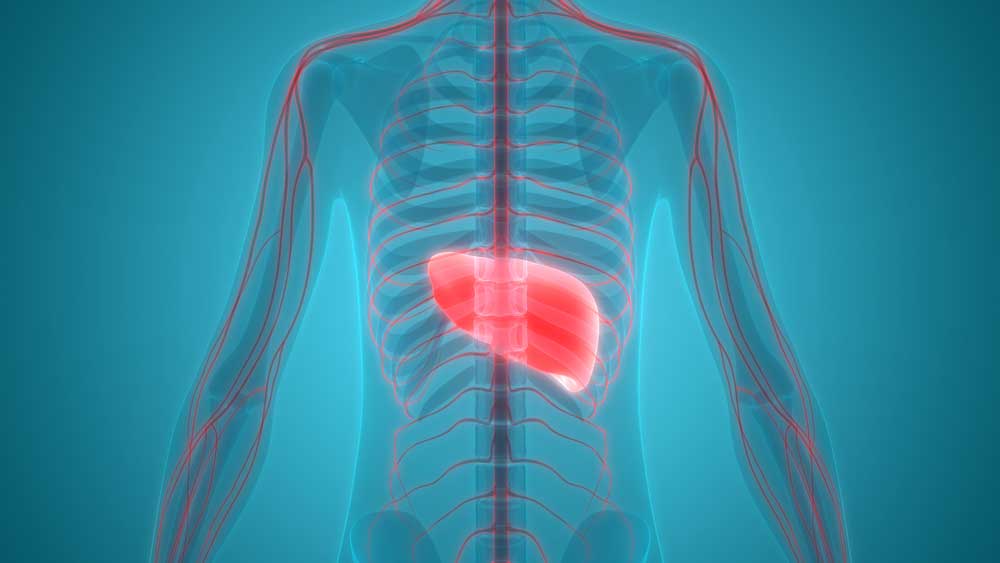
The liver is the second largest organ in the body. Its function is to process everything we eat or drink and filter out any harmful substances from the blood. When there is too much fat in one’s liver, the filtration process is interrupted and can become a health problem.
It is estimated that 25% of the world has Non-alcoholic Fatty Liver Disease (NAFLD), a precursor to NASH or Non-Alcoholic Steatohepatitis. NASH is associated with obesity, cardiovascular disease, type 2 diabetes and metabolic syndrome. It is now the most common liver disorder in the United States and the number one reason for liver transplants.
Starting as Fatty Liver Disease and then progressing to NASH, the buildup of fat in the liver can lead to inflammation of the liver and liver cell damage. Progression of NASH leads to fibrosis or stiffening of the liver and cirrhosis or scarring of the liver. NAFLD and NASH are both silent diseases with few symptoms even if the diseases progress to cirrhosis.
Physicians can monitor liver function blood tests as well as abdominal ultrasounds and liver Fibroscans to determine if you are at risk of developing NAFLD and NASH. However, the only way to definitely determine of you have NASH is to perform a liver biopsy.
The most common treatment for fatty liver disease is weight loss to reduce the fat in the liver. It is estimated that losing up to 3 to 5% of your body weight can help reduce the fat in the liver. Losing 10% of body weight may help reduce inflammation and even fibrosis in the liver. Currently, there are no medications which have been approved to treat fatty liver disease; however, many are in late stage development with promising results.
To learn more about current clinical trial opportunities for fatty liver disease and NASH, please contact us.
Growing up, we’ve all heard the saying, “An apple a day, keeps the doctor away” and in most cases, an apple is a great fruit to eat! However, if you have Crohn’s Disease that might not always be the case. Those afflicted with Crohn’s Disease actually have to peel the skin off of fruits and vegetables with edible skin, however delicious it may be! The skin is an insoluble fiber that can aggravate Crohn’s symptoms causing more gas, bloating, diarrhea and pain. In severe cases, can even cause blockages.
The cause of Crohn’s Disease is still unknown. Scientists believe the cause to be a mixture of environmental, and genetic factors. Crohn’s Disease causes inflammation of the wall of the gastrointestinal (GI) tract. The GI tract is continuous starting at the mouth and ending at the anus. An interesting fact about the GI tract is, it can be considered to be outside of the body. The body changes the environment of the GI tract to be conductive to digesting and absorbing food to the inside of the body. If we followed the journey of the apple discussed earlier after masticating and swallowing the apple is moved down the esophagus, and into the stomach where it will be digested. Next the apple will pass through a sphincter and into the small intestine where the nutrients from the apple will be absorbed. Crohn’s most commonly occurs in the small intestine and during a flare up it is difficult to absorb necessary nutrients before the bolus is moved to the large intestine.
While the small intestine is most commonly affected, with Crohn’s, any part of the GI tract explained above can be affected. The inflammation caused by Crohn’s produces flare ups and can lead to many uncomfortable symptoms. A few of which are: diarrhea, pain, unintentional weight loss, ulcers, malaise, anemia, and anal fissures.
Research has produced many significant advances for Crohn’s Disease, but there are still many unanswered questions. Our research sites are devoted to finding answers to those pressing questions and providing a better outlook for the future of Crohn’s health management. You can be an integral part of shaping the path for future medicine, by participating in a clinical trial.
Ask anyone who has had a Clostridium difficile (C. difficile, or C. diff) infection and they will probably tell you that it was one of the worst experiences of their life. Imagine the worst flu you’ve ever had but on steroids! C. diff is affectionately referred to as “deadly diarrhea” and with symptoms such as watery diarrhea 10 to 15 times a day that’s no joke! It can also come with a multitude of other symptoms such as: severe abdominal pain/cramping, rapid heart rate, fever, blood or pus in the stool, nausea, dehydration, and kidney failure.
What is C. Diff?
C. diff is one of the many different types of bacteria that lives in our intestines. It may sound gross but bacteria in your intestines are completely normal and you need a good balance of them to remain healthy. When something such as antibiotic use throws off the balance in your intestines C. diff may start to grow out of control and begin release toxins that attack the lining of the intestines which leads to that deadly diarrhea.
Is C. Diff contagious?
C. diff is contagious, so even if you were not recently on antibiotics, you can still catch C. diff by contact with a contaminated surface. Spores from C. diff bacteria come from human feces, soil, water and animal feces. These spores can also live for weeks or months outside the body.
Who is at risk?
C. diff is most often associated with doctor or healthcare facility visits or recent antibiotic use. There is a higher risk for adults ages 50 and over, especially those that have frequent doctor visits or have had any type of recent surgery or a hospitalization.
What can you do to lower your risk?
Good handwashing practices, especially after doctor or healthcare facility visits are a great start to lowering your risk of getting a C. diff infection. Another way is to take probiotics daily anytime you take an antibiotic. The reason for this is because when you take an antibiotic it not only kills off the bad bacteria, but it also kills off the good bacteria, giving C. diff a chance to thrive. Taking a probiotic, even if it’s just store bought yogurt, helps feed and rebalance your good gut bacteria. These are not fool proof, but they may help.
A Vaccine to prevent C. Diff?
While Handwashing and probiotics are certainly a must, researchers agree they are still not enough when it comes to preventing this life-threatening infection. Which is why we are involved in a cutting-edge research study working on the development of a new vaccine for C. diff prevention. If you are interested in volunteering, this study is for people ages 50 and up who have been recently hospitalized, have an upcoming surgery, or have frequent healthcare contact. If you are not sure if you qualify, please give our office a call or click below on the site that is closest to your location to sign up and we will be glad to answer any questions!
Fleming Island Center for Clinical Research
904-621-0390
Jacksonville Center for Clinical Research
904-730-0166