We all do things for our parents. Some of us make them a card for their birthday, call them to say hello, or discover key mechanisms behind how the body metabolizes sugar in an attempt to save them from diabetes. Falling into that last category is the first American woman to win a Nobel Prize, Dr. Gerty Cori. She was born to a Jewish family in Prague in 1896. She became a doctor, got married, and worked in research at Carolinen Children’s Hospital. Gerty and her husband, Carl, collaborated and published multiple papers. Central Europe became challenging for Jewish people during the interwar period. She immigrated to the USA with her husband in the 1920s and naturalized in 1928. Her father was diagnosed with diabetes, and it’s said that’s where she got her inspiration. America in the first part of the 20th century was a tough place to be a female researcher. Gerty Cori’s husband was offered prestigious positions that were denied to Gerty based on her gender. Carl Cori would not stop collaborating with his wife and refused positions where Gerty was not welcome. They eventually were hired at Washington University in St. Louis, though Gerty was given a token salary 1/10th of what Carl made. There, Gerty and Carl collaborated and investigated how sugar was broken down and stored in the body. It was said that Gerty had the ideas, and together the husband and wife team made breakthroughs. This culminated in their description of how the body delivers energy to muscles during intense exercise in what came to be called the Cori Cycle. The Cori Cycle is essential to our understanding of how the liver and muscles work together. Our muscles need energy to do anything and everything. Normally, sugar in the form of glucose is broken down using oxygen, releasing energy. During prolonged and/or intense exercise, we can’t get enough oxygen to the muscles fast enough, and they have to produce energy without oxygen. To do this they convert glucose to pyruvate to lactate. Lactate is released into the blood, where it could cause damage if not for the liver. Gerty Cori and her husband’s experiments found that the liver regenerates glucose from the extra lactate. The liver uses more energy to make the glucose than the muscles can generate from it without oxygen, so the Cori Cycle is the shifting of the energy production from the muscles to the liver. Because of this and other critical work illuminating how the body metabolizes glucose, Gerty and her husband shared the 1947 Nobel Prize in Physiology and Medicine, making Gerty the first American woman to win the prize. Earlier that year, Gerty was also finally offered a full professorship at Washington University. She continued her work on glucose metabolism and spent time investigating enzymes and hormones. Her work would later be critical to our understanding of how glucose is regulated through the body, giving targets for diabetes medications. This Women’s History Month, as we honor the remarkable women who have impacted our world, let’s recognize the pioneering spirit of the first American woman to win a Nobel Prize in Physiology or Medicine. Her groundbreaking work laid the foundation for our understanding and treatment of diabetes. We can draw on her inspiration to make our parents proud and continue the legacy of progress and compassion. Staff Writer / Editor Benton Lowey-Ball, BS, BFA
References: National Center for Biotechnology Information (2024). PubChem Pathway Summary for Pathway WP1946, Cori cycle, Source: WikiPathways. Retrieved March 19, 2024 from https://pubchem.ncbi.nlm.nih.gov/pathway/WikiPathways:WP1946. Washington University School of Medicine. (2004). Gerty Theresa Cori. Bernard Becker Medical Library. https://beckerexhibits.wustl.edu/mowihsp/bios/cori.htm Ginsberg, J. (2010). Carl and Gerty Cori and Carbohydrate Metabolism. National Historic Chemical Landmark. https://www.acs.org/education/whatischemistry/landmarks/carbohydratemetabolism.html Gerty Cori – Biographical. (1964). Nobel Lectures, Physiology or Medicine 1942-1962. Elsevier Publishing Company. https://www.nobelprize.org/prizes/medicine/1947/cori-gt/biographical/
Listen to the article here:
GRID VIEW
180 years ago, a doctor in the Austrian Empire conducted a radical experiment that has saved millions of children but cost him his life. This shocking, ground-breaking experiment involved doctors washing their hands. I know, I know, it sounds ridiculous, but doctors not only didn’t wash their hands back then, they were opposed to the very idea so much that the researching doctor was institutionalized and beaten to death. In this article, we’ll explore the history of handwashing, how they came up with the experiment, why people weren’t washing their hands in the first place, why the experiment worked, and how modern hand washing works. Then, we’ll dive into some nitty-gritty science. Handwashing is old. Like, it’s really old. We have good evidence of soap from nearly 3000 years ago. Handwashing as a ritual before meals is in Abrahamic religious texts. It was recorded in ancient Egyptian and Greek civilizations and is even practiced by raccoons. But this was superficial handwashing, mostly meant to get rid of visible dirtiness because we hadn’t discovered germs yet. Instead, ideas of how disease spread were based on things like miasma – the stinkiness of a dirty thing. Ignaz Semmelweis was a physician who, in the 1860s, got a residency in a maternity ward. In those days things were separated by gender, so there were two clinics. One was attended by male doctors and one by female midwives. Dr. Semmelweis noted that people died in the male-run clinic at a rate 300% higher than in the midwife-run clinic. He was appalled and wrote that women would have better outcomes giving birth in the street than in the hospital. The primary disease causing all the deaths was childbed fever, now known as (pew-er-per-al) puerperal fever. Luckily, Dr. Semmelweis had a shocking (shocking!) insight. He theorized that perhaps the fact that the doctors would do autopsies before going to the maternity ward was causing some of the “cadaverous particles” to infect the patients. He got this idea when a fellow doctor cut himself during an autopsy and subsequently died of childbed fever. Dr. Semmelweis concluded that doctors should wash their hands in chlorinated water upon entering the maternity clinic! Within a year the death rate plummeted from ~10% to under 2%. Unfortunately, doctors were reluctant to change their ways. The theory that doctors could be killing their patients was seen as offensive and came with the implication that doctors were unclean, which went against the class system of the era. He was reluctant to release his findings, but when he did they were dismissed and his reputation was ruined. In his book Die Aetiologie, der Begriff und die Prophylaxis des Kindbettfiebers, he is racked with guilt. He was committed to an insane asylum where he was beaten to death by the orderlies within weeks under suspicious circumstances. It would be decades before germ theory gave an explanation for Semmelweis’s findings and brought them back into the public consciousness. He would never know how many millions of children and mothers he saved. In Dr. Semmelweis’s day, they used chlorinated water to wash their hands. Let’s dive into modern-day hand washing. How does washing hands work? Why do we need to wash our hands, even if they look clean? Are there better ways to wash hands? Is hand sanitizer just as good? To start, let’s look at the skin as an immune organ. The skin is awesome. It’s our biggest organ and is the primary defense against invading germs; the tiny microorganisms like bacteria, fungi, and viruses. The skin has three major defense mechanisms. Our immune cells fight organisms that get too close for comfort and our skin hardens and sloughs off, taking bacteria and viruses with it. Before either of those, potential attackers have to deal with the skin microbiome. It turns out our skin isn’t just a cool canvas for tattoos but is an entire ecosystem for thousands and millions and billions of teeny little friends that make a living harvesting our sweat or whatever. Three important genera of bacteria take up the bulk of what we call the resident flora: cutibacterium, staphylococcus, and corynebacterium. These three coat our skin and enhance the immune protection skin gives us. They are commensal organisms, which is kind of like the mob. We give them food and shelter, and they promise to (mostly) do us no harm. They are called “residents” because they live with us our whole lives. They colonize our skin, making it hard for other invaders (called transient flora) to get a foothold. The defense mechanisms they have for themselves work well against the transient flora. In addition, they break down cholesterols we emit into free fatty acids which keep our skin a little acidic, killing invaders. They tend to reside deeper in the skin layers than transient bacteria, are less likely to cause infection, and are harder to remove. This is exactly where handwashing shines. Transient flora, like MRSA, multidrug-resistant gram-negative bacteria, Vancomycin-resistant Enterococci, and “cadaverous particles” tend to be closer to the outer layers of skin and are easier to remove. Effective hand-washing removes the transient flora but keeps the residents intact. Even more effective than just soap and water are antibacterials. These attack the transients in creative ways, degrading the cell walls, DNA, and proteins. Hand sanitizer is effective at destroying many bacteria and can be applied frequently and without a sink. So next time you wash your hands between visiting the morgue and the maternity ward, think of Dr. Semmelweis and thank him for his experimental vision! Staff Writer / Editor Benton Lowey-Ball, BS, BFA
References: Boyce, J. M. (2021). Hand hygiene, an update. Infectious Disease Clinics, 35(3), 553-573. https://doi.org/10.1016/j.idc.2021.04.003 Edmonds-Wilson, S. L., Nurinova, N. I., Zapka, C. A., Fierer, N., & Wilson, M. (2015). Review of human hand microbiome research. Journal of dermatological science, 80(1), 3-12. https://www.sciencedirect.com/science/article/pii/S0923181115300268 Skowron, K., Bauza-Kaszewska, J., Kraszewska, Z., Wiktorczyk-Kapischke, N., Grudlewska-Buda, K., Kwiecińska-Piróg, J., … & Gospodarek-Komkowska, E. (2021). Human skin microbiome: Impact of intrinsic and extrinsic factors on skin microbiota. Microorganisms, 9(3), 543. https://doi.org/10.3390/microorganisms9030543 Semrnelweis, I. (1861). Die Aetiologie, der Begriff und die Prophylaxis des Kindbettfiebers, C. A. Hartleben’s Verlag-Expedition, Translated by K. Codell Carter. Madison, 1983 https://archive.org/details/b28064045 Widmer, A. F. (2000). Replace hand washing with use of a waterless alcohol hand rub?. Clinical infectious diseases, 31(1), 136-143. https://academic.oup.com/cid/article/31/1/136/317796
Listen to the article here:
Last month, the US Food and Drug Administration approved two gene-editing therapies to treat sickle cell disease. This made national news in a way few drug approvals have, but why? What’s the big deal, and why should we care? Sickle cell disease is an inherited genetic disease affecting around half a million babies globally every year. People affected by sickle cell disease have genes that create malformed red blood cells that carry oxygen. These malformed cells become curved like a crescent moon (or a sickle), which results in poor oxygen delivery. Even worse, the curved cells can clump together into clots, which restrict blood flow and cause pain, organ damage, and/or death. Because it is genetic and there has been no known cure, it ranks consistently within the top 20 deaths of children. The disease is most prevalent in people of African descent, and globally the highest concentration of sufferers is in sub-Saharan Africa. Sickle cell disease is a result of problems with genetic mutation and malformed cells, which makes it very hard to target with traditional medicine. In spite of this, innovative researchers have developed two promising treatments for sickle cell disease. These use our own cells to help cure the disease – instead of an oral, topical, or injected medication. These are both gene therapies, where the genetic code of the patient is altered. This is an understandably touchy topic. Gene-editing is different from other medical procedures in that it may be inherited: your genes are passed to your children after all! The benefit of starting gene therapy with sickle cell disease is that we are starting with mutated genes. The mutated sickle-cell-creating genes will already be passed to any children, so fixing the mutations is likely to have better outcomes. I think of it like CPR. With CPR, you are starting with a person who isn’t breathing and has no circulation; you can’t really get any worse than that. With sickle cell gene therapy, as long as the gene-editing tools are specific and target the correct genes it is hard to do worse than one of the top killers of children worldwide. So what are the therapies that were approved? The first, Lyfgenia, is a gene-additive therapy. It uses a modified virus that can’t reproduce to infect cells and add new DNA. The virus, a lentivirus, delivers special RNA to the cells, which our cells incorporate into the DNA strand when they copy it. This genetic code tells the cells to make a different kind of hemoglobin – the protein in red blood cells that carries oxygen. This hemoglobin is a particular type that prevents sticking to the walls of bloodstreams. Note that viruses already deliver RNA that gets encoded into our genes all the time. A 2022 study looked at a protein and found that almost 10% of the human genome may be from viruses. The second therapy, Casgevy, is gene-editing in the most fundamental way. It uses a technology called CRISPR/Cas9 to cut and change pieces of our DNA. While our DNA may be around 10% viral, bacteria have much smaller genomes, and viral insertion of new DNA is a proportionally bigger problem. To combat this, some bacteria have a gene-editing system that can find and remove bits of wayward code. This system was adapted by very smart scientists into a gene-editing tool we can use to find and correct mutations in our genetic code. The process is pretty intense. Blood stem cells are removed from the body, then the CRISPR-Cas9 system edits them outside the body. The modified cells are reinserted into the bone marrow, where they will reproduce and turn into everyday functioning red blood cells. This is mind-blowing. Of course, there is controversy surrounding these therapies. One of the biggest is really unrelated to sickle cell disease, but instead to the very idea of gene-editing. This use of gene therapy in sickle-cell is hard to contest: we’re starting with mutated DNA in blood cells that can kill children. The what-ifs about adding new functionality like laser eyes or super strength get a lot of press and can make us question what it means to be human at a fundamental level. The second big problem is inequality. Could gene-editing be used to make a two-tiered system of wealthy people with great eyesight and perfect skill while poor people suffer? It very much looks like that, as Lyfgenia and Casgevy are both amazingly expensive, somewhere between 2-3 million dollars for treatment. But then, if we can permanently stop sickle cell for a person and all of their descendants, it may be worth it. Staff Writer / Editor Benton Lowey-Ball, BS, BFA
References: Food and Drug Administration. (December 8, 2023). FDA Approves First Gene Therapies to Treat Patients with Sickle Cell Disease https://www.fda.gov/news-events/press-announcements/fda-approves-first-gene-therapies-treat-patients-sickle-cell-disease Milone, M. C., & O’Doherty, U. (2018). Clinical use of lentiviral vectors. Leukemia, 32(7), 1529-1541. https://www.nature.com/articles/s41375-018-0106-0 Frank, J. A., Singh, M., Cullen, H. B., Kirou, R. A., Benkaddour-Boumzaouad, M., Cortes, J. L., … & Feschotte, C. (2022). Evolution and antiviral activity of a human protein of retroviral origin. Science, 378(6618), 422-428. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10542854/ Thomson, A. M., McHugh, T. A., Oron, A. P., Teply, C., Lonberg, N., Tella, V. V., … & Hay, S. I. (2023). Global, regional, and national prevalence and mortality burden of sickle cell disease, 2000–2021: a systematic analysis from the Global Burden of Disease Study 2021. The Lancet Haematology. https://www.thelancet.com/journals/lanhae/article/PIIS2352-3026(23)00118-7/fulltext
Scroll down to listen to this article.
Listen to the article here:
Previously, we explored how the character trait of gratitude can have long-lasting impacts on our health and well-being. Unfortunately, character traits are internal and can be hard to change. Thankfully, scientists are a creative lot and have been working for decades attempting to find out how to increase gratitude. Note that the following methods are still experimental; positive results have been found, but the sample sizes have been relatively small. These interventions have shown increased psychological well-being in the form of increased happiness and satisfaction, as well as fewer depressive symptoms in adults. Please note that this is not a substitute for professional psychological or medical help! Instead, these are interventions that may have positive effects when adhered to. The interventions are: Gratitude journaling, Gratitude letters, Mental subtraction, and Experiential consumption. Gratitude journaling is easy and effective; you just write down things you are thankful for. Various methods have been studied, including the amount (3-5 things) and the frequency (daily or weekly) of journaling. The most effective method I’ve seen is to write three things you are grateful for that happened on the same day. Generally, people wrote a sentence or two about each event. Keeping it limited to daily events helps keep this task from becoming stale. In addition, writing the causes of those events seems to help make the results long-lasting. In one study, a week of gratitude journaling led to increased measures of happiness for the next six months. The idea behind gratitude journaling is that by focusing on the positives, we reinforce those mental pathways and make it more likely that we think about positive things. Gratitude letters are a little more intense than gratitude journaling. In this task, participants write a letter to someone who has been particularly kind to them but hasn’t been properly thanked before. Ideally, the letter should be hand-delivered for maximum effect. By showing gratitude to others, participants had higher scores associated with gratitude themselves. This one is a particularly tactile activity, which may be helpful to some. The effects of this intervention were shown to last over a month on average. Mental subtraction is an interesting intervention. In this activity, participants imagined and wrote about a positive event that occurred in their lives and what their lives would be like had the event never taken place. Alternatively, participants were asked to describe how a positive event was surprising to them, forcing them to think of ways it may not have occurred. This was shown to have positive effects on people’s mental state. By looking at the ways things may not have occurred, it might make people more grateful that they occurred at all. Experiential consumption is an interesting “intervention.” When looking at habits of what people buy, scientists have found that spending money on experiences (trips, music events, etc.) seems to increase people’s happiness and gratitude more than buying tangible items (furniture, clothes, etc.).The thinking behind why experiences may be beneficial is that they are more personal and intrinsic. Experiences are less likely to be compared to others, more likely to be incorporated into who you are, and more likely to be social. Material items are easy to compare to others and unlikely to make lasting impacts on how you see yourself. In addition, ownership is defined as exclusive use, making it an inherently antisocial state. These methods of increasing our gratitude may not be the end-all of increasing our happiness, but they are a good start. We have a few tips to increase the success rate of these interventions. First, a desire for self-improvement helps a lot. If you want to be more thankful this season, it will make each of these tasks easier. Second, expectations matter. The benefits of these interventions may not change your life, but they are pretty sure to improve how you feel about it; plus, they are basically no-risk (unless your experiential consumption is skydiving). Finally, it is easier to follow through on engaging activities. Things like writing the causes of a thankful event may help keep things engaging and fun, making you more likely to complete the task. Feel free to modify these as needed to keep yourself engaged and having fun with them. Hopefully, these ideas help increase your gratitude this Thanksgiving season. Thank you, as always, for reading! Staff Writer / Editor Benton Lowey-Ball, BS, BFA
References: Allen, S. (2018). The science of gratitude (pp. 1217948920-1544632649). Conshohocken, PA: John Templeton Foundation. https://ggsc.berkeley.edu/images/uploads/GGSC-JTF_White_Paper-Gratitude-FINAL.pdf Dickens, L. R. (2017). Using gratitude to promote positive change: A series of meta-analyses investigating the effectiveness of gratitude interventions. Basic and Applied Social Psychology, 39(4), 193-208. https://www.tandfonline.com/doi/full/10.1080/01973533.2017.1323638 Enmons, R. A., & McCullough, M. E. (2003). Counting blessings versus burdens: An experimental investigation of gratitude and subjective well-being in daily life. Journal of Personality and Social Psychology, 84(2), 377-389. Geraghty, A. W., Wood, A. M., & Hyland, M. E. (2010). Attrition from self-directed interventions: Investigating the relationship between psychological predictors, intervention content and dropout from a body dissatisfaction intervention. Social science & medicine, 71(1), 30-37. https://doi.org/10.1016/j.socscimed.2010.03.007 Kaczmarek, L. D., Kashdan, T. B., Kleiman, E. M., Baczkowski, B., Enko, J., Siebers, A., … & Baran, B. (2013). Who self-initiates gratitude interventions in daily life? An examination of intentions, curiosity, depressive symptoms, and life satisfaction. Personality and Individual Differences, 55(7), 805-810. https://doi.org/10.1016/j.paid.2013.06.013 Koo, M., Algoe, S. B., Wilson, T. D., & Gilbert, D. T. (2008). It’s a wonderful life: Mentally subtracting positive events improves people’s affective states, contrary to their affective forecasts. Journal of personality and social psychology, 95(5), 1217. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2746912/ Renshaw, T. L., & Olinger Steeves, R. M. (2016). What good is gratitude in youth and schools? A systematic review and meta‐analysis of correlates and intervention outcomes. Psychology in the Schools, 53(3), 286-305. https://onlinelibrary.wiley.com/doi/10.1002/pits.21903 Seligman, M. E., Steen, T. A., Park, N., & Peterson, C. (2005). Positive psychology progress: empirical validation of interventions. American psychologist, 60(5), 410. https://doi.org/10.1037/0003-066X.60.5.410 Walker, J., Kumar, A., & Gilovich, T. (2016). Cultivating gratitude and giving through experiential consumption. Emotion, 16(8), 1126. https://doi.org/10.1037/emo0000242
Scroll down to listen to this article.
Listen to the article here:
Clinical research has many benefits. There are the obvious ones, like a stipend for time and travel and the potential benefits of an investigational medication, but also more esoteric benefits, like increased quality of care, attention from medical staff, and knowledge about the conditions people face. We recently had a chance to talk with one of our repeat patients, Brendle, who will walk us through her clinical research experience and why she keeps signing up for more studies. “I’ve learned so much,” she stated. One of the big benefits of clinical research is the knowledge gained through experience. Brendle said “Dr. Koren explains things so well.” Not only do patients get access to podcasts from Dr. Michael Koren and articles from our knowledgeable staff, but they also get a lot of direct face-to-face time with medical professionals and support staff. Transparency is key in clinical research, so we spend a lot of time talking through the full medical history of every patient. We also make sure everyone understands the science, risks, benefits, and process of a trial before enrolling. We typically schedule an hour or two for patients to talk through medical history, medications, and the specifics of a clinical trial before enrolling. Compare this to a typical doctor’s visit with a wait time of 15-30 minutes and only 10-20 minutes of time with a doctor and it’s easy to see why people like Brendle enjoy the clinical trial experience so much. Imagine how many complications could be avoided if primary care practices were able to spend an hour with each patient before prescribing a new medication! Of course, medications and procedures are the major benefit most people think of when it comes to clinical research. Participants rank risks and benefits as the most important information before participating. The importance of understanding the potential risks of investigational medications or procedures should not be taken lightly. We ensure that patients are given the information needed to make well-informed decisions. Obviously, potential benefits are different in every study. Registry studies only collect information, and the benefit is in drug development down the road (and compensation). Phase 3 studies, in contrast, can have long-lasting effects on biological markers of health. Brendle notes, “when I first came here, my Ejection Fraction (EF) was only 10%. Now it’s up!” This information is exactly what we want to know for statistical analysis, but the real-world consequences can be even better. Brendle continues, “I could only go from the bed to the couch and back, but now I can do much more.” Amazingly, it’s possible that benefits like this may be realized even when a patient is given a placebo. Not only is the placebo effect real, but the increased attention from doctors and medical staff makes sure we catch any health changes as soon as they happen. Brendle finished up her chat with us saying “This is the best experience. I am thankful to get into studies.” We are very thankful for patients like Brendle – and you, dear reader – who help push science forward by volunteering for clinical trials! Staff Writer / Editor Benton Lowey-Ball, BS, BFA
References: Business Wire, (March 22, 2018). 9th annual vitals wait time report released https://www.businesswire.com/news/home/20180322005683/en/9th-Annual-Vitals-Wait-Time-Report-Released CISCRP, (2021). Perceptions and insights study 2021. https://www.ciscrp.org/services/research-services/perceptions-and-insights-study/ Tai‐Seale, M., McGuire, T. G., & Zhang, W. (2007). Time allocation in primary care office visits. Health services research, 42(5), 1871-1894. https://doi.org/10.1111%2Fj.1475-6773.2006.00689.x
Scroll down to listen to this article.
Listen to the article here:
It was the best of me, it was the worst of me. There are two versions of your dear author: the one who loves cookies, pizza, and video games and the one who loves surfing, cycling, and roasted vegetables. In a stroke of complete luck, I live at the beach where exercise and healthy living are trendy and encouraged. That wasn’t always the case, however. When I was younger, I went to college in Indiana. There was no beach, I had no bike, everyone had a computer, and my meal plan included unlimited pizza. Unsurprisingly, these two versions of myself have very different health outcomes. One lifestyle is associated with heart attacks, diabetes, and obesity, while the other isn’t. Which version makes it through to the end isn’t just determined by self-discipline and genetics but heavily by the community you are in. Things that contribute to your health outcomes are called determinants of health. These include your genetics, behavior, and medical care, but also the physical place you spend time and social factors. The determinants of health aren’t insulated; they interact and influence each other. That last one is properly termed Social Determinants of Health (SDOH). These are the daily interactions with people and the area around you, but also the bigger systems that influence these interactions. Examples of the social determinants of health include: It was easy to see these social determinants at work during the pandemic. The “Quarantine 15” was a real phenomenon where somewhere around 48% of people in America gained weight. People were stressed, jobs and income were unstable, healthcare access was limited, exercise options dropped, and – importantly – many of us lost our community connections. Luckily, with the pandemic calming down, we are presented with opportunities to shore up our social determinants of health. With the pandemic as a reference, we can see that social determinants of health are subject to very big forces. To improve the social determinants of health in our area, we would ideally look at inequality, structural biases, macroeconomic conditions, and government policy. On the personal level, the most productive changes we can make (other than moving halfway across the country) are at the community level. This includes your family, friends, neighbors, and people you interact with and share common ground with, such as those in a book club or church. From a healthcare perspective, “community” determines who you talk to when sick, who checks in on you, who cooks food when you have a newborn, who takes you to the doctor when you can’t drive, and so on. Luckily, your community can expand. When you join a clinical trial at one of our ENCORE Research Group sites, you don’t just gain access to cutting-edge research, you gain a community that is committed to health. We partner with other groups, perform community outreach, and write extremely well-written, clever, and funny articles for your inbox weekly. On top of this, when enrolled in a clinical trial, we need to monitor your health and stay in touch. We look for what will help your specific situation and if you miss an appointment we reach out to make sure you are ok. ENCORE stands for Encouraging COmmunity Research and Education, it’s right there in our name! Staff Writer / Editor Benton Lowey-Ball, BS, BFA
References: Khubchandani, J., Price, J. H., Sharma, S., Wiblishauser, M. J., & Webb, F. J. (2022). COVID-19 pandemic and weight gain in American adults: A nationwide population-based study. Diabetes & Metabolic Syndrome: Clinical Research & Reviews, 16(1), 102392. https://doi.org/10.1016%2Fj.dsx.2022.102392 Artiga, S., & Hinton, E. (2018). Beyond health care: the role of social determinants in promoting health and health equity. Kaiser Family Foundation, 10. https://www.kff.org/racial-equity-and-health-policy/issue-brief/beyond-health-care-the-role-of-social-determinants-in-promoting-health-and-health-equity/ Baciu, A., Negussie, Y., Geller, A., Weinstein, J. N., & National Academies of Sciences, Engineering, and Medicine. (2017). The Role of Communities in Promoting Health Equity. In Communities in Action: Pathways to Health Equity. National Academies Press (US). https://www.ncbi.nlm.nih.gov/books/NBK425849/ Centers for Disease Control and Prevention. (8 December, 2022). Social determinants of health at CDC. U.S. Department of Health & Human Services. https://www.cdc.gov/about/sdoh/index.html
Scroll down to listen to this article.
With contributions from Stacey Lowey-Ball, BA AnthropologyListen to the article here:
You may have heard the news; earlier this month an FDA committee unanimously concluded that phenylephrine, a common decongestant, doesn’t work. What does this mean? Why is it still on shelves? Is it poison? Should I throw my medicine away? Is the FDA a scam!? What’s the point of science if they change the rules?!? We’ll address the last two questions first. Good science is a process of change. It’s not definitive; just our best, evidence-based guess at how to predict what will happen given current best experimentation and data. As we get more data of better quality the conclusions drawn by scientists change. To be clear, when scientists update their conclusions this is good and means science is working. It means we are getting more accurate information through better practices and updated information. New technology plays a big part in this. Think of it like maps. The first explorer to document an area may have a hand-drawn map outlining the major features. Later cartographers may come along and refine the map, making it more accurate and filling in the details. Their map may show a landmark in a different, more accurate position. This doesn’t mean the original mapmaker was malicious, or that maps don’t work, but instead that we can update our information to have a more accurate view of the world. Back to the issue at hand, let’s find out what we’ve learned. On September 11th and 12th, 2023, the Non-prescription Drug Advisory Committee reviewed the results of several clinical studies which looked into the effectiveness of oral phenylephrine at lowering nasal congestion (stuffy nose). These studies measured symptoms in hundreds of patients who took phenylephrine and/or a placebo sugar pill in controlled environments. These studies found, by and large, that the decongestant was not significantly better than the placebo at providing relief. It should be noted that in the studies, most patients found relief from both phenylephrine and the placebo! It should also be noted that participants had few or no adverse reactions to the studies, though some had headaches. In response, the committee concluded that phenylephrine is not effective at providing relief when compared with a placebo; the drug doesn’t work. So what does this mean for me? First, note that this is an advisory committee. They provide independent advice to the FDA, but do not make policy. In the near term nothing has changed. The FDA will likely take a while to make any policy changes and may have public input. Additionally, the clinical trials did not find the medication dangerous, just ineffective. This means phenylephrine isn’t dangerous at the recommended doses; you don’t need to throw it away (unless it’s expired!). It also means that a phase-out period will probably be slow, because there isn’t a danger to the public beyond wasting money on a medicine that works no better than a placebo. Finally, how did this happen? How did a medication that doesn’t work get past the FDA? The answer is that while oral phenylephrine doesn’t seem to provide relief, inhaled phenylephrine continues to show effectiveness! When the oral form was approved in the 1970s, scientists thought around 30% of the medication would be absorbed in the gut. It has come to light that around 1% of the decongestant medication is actually available for our body to use when taken orally. From this, it follows that we would need to take much higher doses to get significant relief, which comes with increased side effects – including to the heart! On top of this is the completely fascinating finding in 2015 that placebos are getting better. A meta-study of several placebo-controlled clinical trials found that the effects of medications stayed the same, but the effect of placebos has been increasing over time! Some scientists believe this may be because we expect medications to do more, so the placebo is more effective! This means that when clinical trials are repeated, medications have a more difficult time showing effectiveness versus placebo. Think of our map-makers. That same landmark may have been perfectly mapped by cartographers, but tectonic plates can still cause it to slowly shift position. Lucky for us this means that new medicines brought to market are virtually guaranteed to be more effective than if they were introduced last century! Staff Writer / Editor Benton Lowey-Ball, BS, BFA
References: Division of Nonprescription Drugs 1 (DNPD1), Division of Inflammation and Immune Pharmacology (DIIP), Office of Clinical Pharmacology (OCP), Division of Epidemiology II (DEPI-II). (September 11, 2023). Efficacy of Oral Phenylephrine as a Nasal Decongestant. U.S. Food & Drug Administration. https://www.fda.gov/media/171915/download U.S. Food & Drug Administration. (September 14, 2023). FDA clarifies results of recent advisory committee meeting on oral phenylephrine. U.S. Food & Drug Administration. https://www.fda.gov/drugs/drug-safety-and-availability/fda-clarifies-results-recent-advisory-committee-meeting-oral-phenylephrine Meltzer, E. O., Ratner, P. H., & McGraw, T. (2015). Oral phenylephrine HCl for nasal congestion in seasonal allergic rhinitis: a randomized, open-label, placebo-controlled study. The Journal of Allergy and Clinical Immunology: In Practice, 3(5), 702-708. https://pubmed.ncbi.nlm.nih.gov/26143019/ Meltzer, E. O., Ratner, P. H., & McGraw, T. (2016). Phenylephrine hydrochloride modified-release tablets for nasal congestion: a randomized, placebo-controlled trial in allergic rhinitis patients. Annals of Allergy, Asthma & Immunology, 116(1), 66-71. https://doi.org/10.1016/j.anai.2015.10.022 National Library of Medicine. (March 3, 2011). Safety Study Comparing Phenylephrine HCL Extended Release Tablets 30 mg and Placebo (Study CL2007-07)(P07529)(COMPLETED). U.S. Department of Health and Human Services.ClinicalTrials.gov ID NCT00874120. https://clinicaltrials.gov/study/NCT00874120?tab=results Tuttle, A. H., Tohyama, S., Ramsay, T., Kimmelman, J., Schweinhardt, P., Bennett, G. J., & Mogil, J. S. (2015). Increasing placebo responses over time in US clinical trials of neuropathic pain. Pain, 156(12), 2616-2626. https://doi.org/10.1097/j.pain.0000000000000333
Scroll down to listen to this article.
Listen to the article here:
Clinical research is vital in developing knowledge geared toward improving future health practices. It is often the only feasible solution to medical conditions where standard treatment has failed. Research can be groundbreaking and progressive but study populations lack diversity, especially regarding demographics such as race, ethnicity, age, and sex. Which begs the question: “Why is diversity important to research?” Simply put, various subsets of people can process the same medication differently. Through the clinical research process (guided by strict safety protocols), researchers gather data on how participants experience the same investigational product (IP). Suppose a clinical trial includes people from many different age, gender, and racial/ethnic groups. In that case, researchers will then have data on how several groups of people respond to the same product based on those differences. When these new products reach the market, doctors will know what works best, what doesn’t, and for whom based on those findings. Through research, doctors learned that it is best to prescribe particular medications based on patients’ ethnicity/racial background when treating hypertension. As we move forward, the clinical research community thrives on increasing the participation of all minority age, gender, and racial/ethnic groups to improve the safety profile of medical products. The US government must lead this effort through legislation. At ENCORE, we recognize that to benefit the communities we serve, we must take the steps necessary to best represent ALL in the trials we conduct. However, this requires overcoming numerous challenges, including long-standing mistrust and economic barriers which prevent minority groups from accessing and participating in research. Even though clinical trials have evolved from historically unethical practices involving minority racial groups to a transparent process where participant safety and protection are paramount, there is still a significant lack of trust on the part of potential study subjects. Especially for those who are dubious, establishing credibility and integrity within clinical research practice is crucial to growing minority group participation. We believe that physicians, especially those who serve ethnically/racially variant communities, play a significant role in achieving Diversity in clinical trials by bridging trust between researchers and minority participants. ENCORE physicians have dedicated their efforts to working alongside primary care physicians and specialists who serve these communities; to provide them with research material relevant to their practice. Doctors then have the information to make informed recommendations on whether a particular clinical trial is appropriate for their patients. Not only are people more likely to be confident in the recommendations coming from their doctors, but doctors find themselves better prepared to help patients who have failed on current therapeutic approaches. Unlike when seeking intervention via traditional means, economic hindrance isn’t a preventative factor when one chooses to participate in clinical research. Healthcare costs are a significant burden to many; however, all of the investigational medical products available here at ENCORE cost our patients nothing. All study-related materials, evaluations, blood tests, and imaging are done for free. Study participants will never be billed. Sponsors such as pharmaceutical companies, governments, and foundations fund medical research through study grants. Grants provide the funding to conduct studies at local research sites, so the cost is not transferred to the volunteers. This allows people experiencing financial constraints or without health insurance the opportunity to receive potentially groundbreaking medical treatment at no cost to them. A small monetary compensation is often provided for participants’ time and inconvenience associated with participating in a clinical study. Payment is kept within a reasonable amount to prevent enticement and undue influence on participants. Despite these steps, we recognize that much more needs to be done to garner diverse research participants in all our trials. Appropriately representing Diversity in clinical trials is an ethical and medical obligation that bounds all stakeholders. Critical players like research sponsors, investigators, referring physicians, coordinators, recruiters, and patients must work collaboratively to achieve this goal. A multi-level stakeholder approach can be more successful than one which addresses a single barrier or involves individual stakeholders. As a research facility, our responsibility in achieving increased Diversity amongst trial participants will build on our investments towards nurturing long-standing relationships. These relationships are between sponsors, community members, our diverse pool of staff and physicians, and our commitment to engagement and learning from diverse patient groups. With this approach, we are confident that trial enrollment will continue to become more diverse and result in a more accurate representation of the people that products are intended to treat. Albertha V. Lalljie, MBBS, MPH
We humans seem to like making a fresh start. Whether it’s the beginning of a semester, a month, or a week, we like having a “clean slate” to make changes. The most widely used of these fresh start times are at the beginning of the year, with a New Year’s Resolution. Over 40% of all Americans make New Year’s resolutions, but much like a firework, we make a bright claim with a loud noise, only for it to burn out quickly as the year goes on. How can we make good resolutions that we are likely to follow, and are there strategies we can use to help us follow through? Probably the most important piece of a New Year’s Resolution is coming up with a good resolution in the first place! Surveys show that around two-thirds of all resolutions are health-oriented, including eating healthier, exercising, getting in shape, etc. Psychological studies have shown that the wording of your resolution matters. Most resolutions can be broadly lumped into either activation or avoidance goals. Activation goals are those that encourage you to do something: exercise more, eat more greens, etc. Avoidance goals are those that encourage you to not do something: watch less TV, eat less pizza, etc. Several studies have shown that activation goals are significantly more likely to be successful than avoidance goals Sometimes our end goal is to decrease something: to lose weight, stop smoking, or eat slightly fewer cookies. In order to increase chances of success, it can be helpful to reimagine these goals as activation goals. Instead of losing weight, we can aim to exercise four days a week. Instead of stopping smoking, we can try to chew gum daily. Instead of eating fewer cookies, we can try to do some push-ups instead. When trying to avoid negative things, it can be hard to find rewards and easy to identify failures. By trying to do positive things, we can enjoy the reward of achieving our goal incrementally. Even small changes can help. Instead of “I resolve to eat no cookies this year” we can set the goal as “I resolve to do a push-up instead of eating a cookie every day.” Eventually, we will focus more on the positive action, the push-up, than the negative one, the cookie. This way our brain will spend more time focusing on the things we resolve to do! When we follow through on a resolution, we are making a behavioral change. These changes are governed by our brain, and mimic changes within it. Some of our most popular resolutions correspond to changes in our reward pathway, called the mesocorticolimbic circuit. This contains several brain structures and is a part of the brain that is hijacked by addictive drugs. Two structures in particular, the nucleus accumbens and striatum, seem to be affected by things like resolutions. Addictive things including sugar decrease these areas’ sensitivity to naturally occurring dopamine. This makes the brain need more and more of those items to find the same level of reward. Lowering sugar, drugs, and alcohol can help restore the dopamine receptors and give your brain a fighting chance. Studies have also shown that exercise increases dopamine sensitivity of the mesocorticolimbic circuit, giving some protection against addictive undesirable behaviors. Other behaviors that we do frequently and repetitively will also make changes to the brain’s pathways, reinforcing the behaviors. So now we know how to structure our resolutions, and how our brain responds to changes, but what can we do to make sure we don’t give up on our resolutions? The most important change is a lifestyle change. This is true with resolutions, but also with weight loss medications, smoking cessation, etc. Changing the triggers for what you want to avoid makes it easier to do the activities you desire. Even small changes – like sitting in a different chair than your preferred cookie-binge recliner – can make the process easier. Along with this, we want to make sure we have strategies to deal with tempting situations. If work has cookies on Fridays, drinking a lot of water can fill your stomach and help alleviate the temptation. Unexpected situations can also arise. If your mother invites you for afternoon tea and biscuits – only for you to learn that “biscuit” is British for “cookie”- having a plan to politely decline can be very handy. Finally, realize that resolutions aren’t all-or-nothing. If I succumb to chocolatey chip temptation and eat a cookie today, it doesn’t mean I’ve failed at my resolution and should give up. Instead of looking at hiccups as failures, look at them as learning opportunities. These are great opportunities to learn what triggered your lapse and practice a strategy to act positively and avoid this trigger in the future. Taken together we have solid starting points for our resolutions. Resolve to do positive actions that you want to accomplish. Structure resolutions to be activation based and give yourself opportunities to celebrate success instead of regretting failure. Give yourself the advantage of changing your lifestyle to accommodate and incentivize your resolution. Give yourself a break when you miss a day and learn how to move forward better tomorrow. When we resolve to do things we want to do, we only have to countdown the days until we celebrate another New Year and a successful resolution! Written by Benton Lowey-Ball, BS Behavioral Neuroscience
Sources: Larimer, M. E., Palmer, R. S., & Marlatt, G. A. (1999). Relapse prevention. An overview of Marlatt’s cognitive-behavioral model. Alcohol research & health : the journal of the National Institute on Alcohol Abuse and Alcoholism, 23(2), 151–160. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6760427/ Oscarsson, M., Carlbring, P., Andersson, G., & Rozental, A. (2020). A large-scale experiment on New Year’s resolutions: Approach-oriented goals are more successful than avoidance-oriented goals. PLoS One, 15(12), e0234097. https://doi.org/10.1371/journal.pone.0234097 Trifilieff, P., & Martinez, D. (2014). Imaging addiction: D2 receptors and dopamine signaling in the striatum as biomarkers for impulsivity. Neuropharmacology, 76 Pt B(0 0), 498–509. https://doi.org/10.1016/j.neuropharm.2013.06.031 Wimmer, S., Lackner, H. K., Papousek, I., & Paechter, M. (2018). Goal orientations and activation of approach versus avoidance motivation while awaiting an achievement situation in the laboratory. Frontiers in psychology, 9, 1552. https://doi.org/10.3389/fpsyg.2018.01552
Listen to the article here:
Most of us have heard by now that chocolate is healthy, or that a small amount is healthy, or that you can eat an infinite amount of chocolate and it will be healthy forever. Where do these claims come from, and do they add up? There is evidence of people consuming chocolate up to 1600 years ago. It is native to the Americas and was said to be the “food of the gods” in mesoamerica. Today we think of chocolate as sweet and delicious and the perfect food, but this was not always the case. Chocolate is thought to have originally been mixed with water and drunk as a bitter, spiced beverage. During the 1500’s chocolate was brought to Europe, where it was considered as exotic as Mars. Healers claimed chocolate healed diseases of the liver and stomach, and that it could help with fever. By 1631, chocolate had changed. Adding sugar was now typical, and the prescriptions for chocolate had changed as well. Chocolate in this era was used to help gain weight (likely due to sugar), stimulate the brain (likely due to caffeine), and aid in digestion. Ironically, the same benefits chocolate seemingly presented to chronically underweight pre-industrial people has become a bit of a problem for us. By the mid to late 1800’s there were investigations into the health problems associated with chocolate’s additives – milk and sugar. They found that regularly eating fatty, sugary foods might not be healthy. By the 1900’s chocolate began to be associated with obesity, tooth decay, gum disease, etc. The “dark” chocolate age had begun. By the early 2000’s, the opinion pendulum on chocolate had begun to swing back. Individual components of chocolate, such as flavanols, methylxanthines (Methyl-zan-theens) and polyphenols were shown to be beneficial to heart function in a lab. Since then there have been claims that chocolate helps everything from cardiovascular problems to metabolic ones and even cancer. It looked like chocolate was on a holiday high in medical opinion. Unfortunately, these results may have been candy-coated. Research trials haven’t shown as much benefit as in the lab. One sweet spot picked up by newspapers was an observational meta-study which looked at over 300,000 participants. This study looked for an association between chocolate consumption and coronary artery disease (CAD). They found that people who ate chocolate more than once a week (or more than 3½ times a month) had a significantly lower incidence of CAD, heart attack, heart failure, and acute coronary syndrome. It is important to note that this was not an interventional study, and only looked at associations. Additionally, this didn’t take into account the type of chocolate eaten. Finally, this study found that some negative indicators actually rose, likely due to the extra calories from fats and sugars added to chocolates. The best way to look for health benefits or drawbacks of any medicine is to do an interventional experiment – a clinical trial. This is where you compare groups randomly assigned to take chocolate or a placebo. An examination of 15 such studies where chocolate was the medicine sadly found few benefits. These studies looked for changes in: When looking at all 15 studies, there was no significant change in any of these indicators. The only significant change across studies was a decrease in triglycerides. This can be helpful, as high triglycerides can be a risk factor for CAD, stroke, and pancreatitis. Overall, however, chocolate doesn’t appear to be the miracle drug it’s been touted as for the last millennium and a half. As we have learned countless times, using randomized clinical (interventional) trials is the best and often only way to discover if medicines have the effects people claim! Interventional trials are conducted at clinical research organizations such as ours, ENCORE Research Group. We are a premier clinical research organization that has conducted more than 2,500 clinical trials over 25 years and has worldwide recognition for providing patients access to cutting edge medical research. Written by Benton Lowey-Ball, BS Behavioral Neuroscience
Sources: Krittanawong, C., Narasimhan, B., Wang, Z., Hahn, J., Virk, H. U. H., Farrell, A. M., … & Tang, W. W. (2021). Association between chocolate consumption and risk of coronary artery disease: a systematic review and meta-analysis. European journal of preventive cardiology, 28(12), e33-e35.https://doi.org/10.1177/2047487320936787 Lippi, D. (2015). Sin and pleasure: the history of chocolate in medicine. Journal of agricultural and food chemistry, 63(45), 9936-9941. Montagna, M. T., Diella, G., Triggiano, F., Caponio, G. R., Giglio, O. D., Caggiano, G., … & Portincasa, P. (2019). Chocolate,“food of the gods”: History, science, and human health. International Journal of Environmental Research and Public Health, 16(24), 4960. https://doi.org/10.3390/ijerph16244960 Tan, T. Y. C., Lim, X. Y., Yeo, J. H. H., Lee, S. W. H., & Lai, N. M. (2021). The health effects of chocolate and cocoa: A systematic review. Nutrients, 13(9), 2909. https://doi.org/10.3390/nu13092909
Listen to the article here:
Several of my friends hate flossing their teeth. They go months without flossing, which I think is pretty gross. But then an odd thing happens. About a week before their dental appointment, these same friends will start flossing. By the time they reach their appointment, they have unusually clean gums (though dentists can see through this fairly well, I’m told). On a different tone, some family members have a condition called White Coat Syndrome. When they go to the doctor’s office, their nervousness causes a spike in blood pressure or heart rate, giving deceptively high readings. What’s going on? Can psychological effects like these be used to our advantage?
The Hawthorne Effect is a term used to describe a very beneficial effect seen in clinical trials. This is named after a productivity study in Hawthorne Works, a Western Electric factory in the 1920s and 30s. The study was attempting to discover a link between the amount of light and productivity of workers. When increasing the amount of light, productivity increased. Strangely, when lowering the amount of light, productivity also increased! Researchers attributed the increase in productivity to the workers simply being observed. In research, we tend to see increased positive results for patients simply because we are observing them in a study.
Hawthorne Works
Let’s analyze a 2014 sleep study. Researchers measured 195 patients’ amount and quality of sleep at night. 81 days later, before any medical intervention, researchers measured the patients again. They found that patients slept an average of 30 minutes longer per night and had an increased quality of sleep. This was before any medication or intervention! The change was attributed to the Hawthorne Effect. Patients at ENCORE Research Group comment on the excellent quality of care they receive during clinical trials. Instead of seeing a doctor for a few minutes once a year, patients see doctors and medical staff for much longer and are encouraged or required to call and report changes in health. Quality of care is increased and makes for a pleasant and healthful patient experience. Patients in clinical trials may also experience more observation time from medical professionals due to the attention to detail that clinical trials require for data integrity in studies. Finally, patients are found to have better adherence to medication requirements while undergoing clinical trials. The increased emphasis on accuracy and adherence results in better patient outcomes, even when they are part of a placebo or standard-of-care group. In clinical trials, we see these benefits and must account for them. Randomization of patients helps spread the effect. Everyone sees increased baseline results on average; we are interested to find out if those receiving investigational treatment do even better. Join a clinical trial today and experience the Hawthorne Effect for yourself… and floss your teeth! Written by Benton Lowey-Ball, BS Behavioral Neuroscience
Sources: Benedetti, F., Carlino, E., & Piedimonte, A. (2016). Increasing uncertainty in CNS clinical trials: the role of placebo, nocebo, and Hawthorne effects. Lancet Neurol, 15, 736-47. http://dx.doi.org/10.1016/S1474-4422(16)00066-1 Cizza, G., Piaggi, P., Rother, K. I., Csako, G., & Sleep Extension Study Group. (2014). Hawthorne effect with transient behavioral and biochemical changes in a randomized controlled sleep extension trial of chronically short-sleeping obese adults: implications for the design and interpretation of clinical studies. PLoS One, 9(8), e104176. https://doi.org/10.1371/journal.pone.0104176 ENCORE Research Group. (2020, October 14). Hawthorne effect.[Video]. Youtube. https://www.youtube.com/watch?v=1DH7jwqFlyw Mayo, E. (1993). The human problems of an industrial civilization. The Macmillan Company. McCarney, R., Warner, J., Iliffe, S., Van Haselen, R., Griffin, M., & Fisher, P. (2007). The Hawthorne Effect: a randomised, controlled trial. BMC medical research methodology, 7(1), 1-8. https://doi.org/10.1186/1471-2288-7-30
Listen to the article here:

In science and medicine we measure if and how well things work using measurements. This idea may sound simple, but it’s often a challenge to find out exactly what to measure – and how. We typically measure things that can change – things that can vary. We call these things variables. Variables can be broadly split into two major categories: dependent and independent. Either type of variable can change, the difference is what changes them. Independent variables are changed by researchers, particularly in clinical (patient) research. This variable in a medical research study is what we are testing. The changes to an independent variable may include dose, length, and method of drug delivery. We evaluate independent variables that may change outcomes of the people in a study – but sometimes they do not. In order to understand the effect of medicines, researchers test the medicine against a control. The control could be a placebo (something that has no effect) or a standard of care (the current normal medicine). Dependent variables are what we expect to change during a trial. In a clinical research, we may expect changes in blood pressure, cholesterol levels, disease symptoms, mortality, and other categories. In a well designed study, we assess changes in the dependent variables related to changes in the independent variables. There is always the chance that the dependent variables are changed by other things, however. A patient might take a new blood pressure medicine but retire from their job. The reduced stress could decrease their blood pressure even if the medicine did not. Because of individual changes in people’s circumstances, researchers use statistics to find trends. If your blood pressure medicine was only studied on the one person above, you might have erroneous results. Instead clinical trials have dozens, hundreds, or even thousands of participants. With large populations these little differences get figured out. One person might retire, but another might get fired, having an opposite effect. Altogether, statistical analysis can help discover if any changes in the dependent variable are due to the effects of the independent ones.
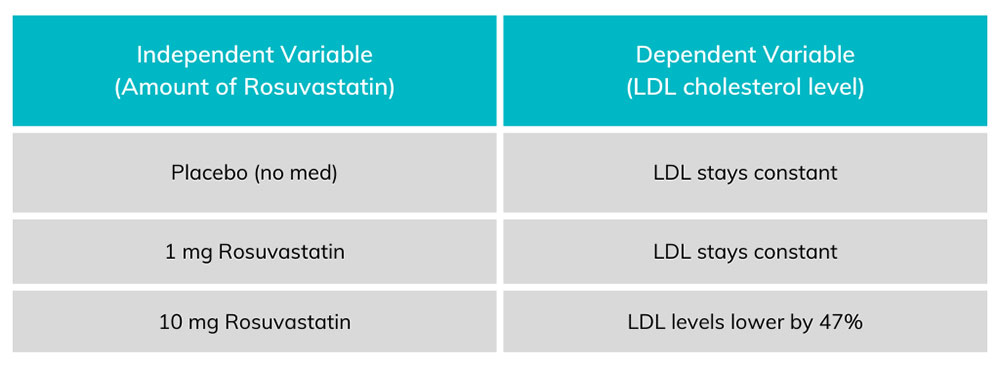
Chart 1. Each amount of Rosuvastatin on the left corresponds to an amount of LDL on the right. The dependent variable (LDL levels) change in proportion to the amount of independent variable (rosuvastatin) taken by the patient.
Other variables exist in a study. The most concerning of these variables is known as a confounding variable. This is a variable that can undermine the study at a fundamental level. A confounding variable can be introduced by researchers and might include things like placing all overweight patients in the 10 mg group and all underweight people in the placebo group. ENCORE Research Group (and any legitimate clinical research group) avoids confounding variables and bias by randomizing patients. Patients are randomized through an impartial method (usually a computer program) which will randomly place patients into any of the test groups. By randomizing patients, we can avoid the most concerning confounding variables and make sure we are studying what we intend to! To learn more about the clinical trial process, call our Recruitment Team at (904) 730-0166. Written by Benton Lowey-Ball, BS Behavioral Neuroscience
Sources: Schweiger, C. (2003). Clinical trials with rosuvastatin: efficacy and safety of its use. Italian Heart Journal: Official Journal of the Italian Federation of Cardiology, 4, 33S-46S. https://pubmed.ncbi.nlm.nih.gov/14983745/ Stewart, P. A. (1978). Independent and dependent variables of acid-base control. Respiration physiology, 33(1), 9-26. https://www.nlm.nih.gov/nichsr/stats_tutorial/section2/mod4_variables.html
Listen to the article here:
My buddy recently bought an e-bike on the internet. It has an enormous battery, goes pretty fast, and is salt air resistant – an important feature at the beach. It’s the perfect bike. Or at least it would be, except it is still on a dock in China, waiting for a cargo ship to deliver it. The bike is no good if it can’t get to where it needs to be. The same is true of drugs: a drug is only as good as its delivery system. Usually, the “buyer” of a drug is a cell somewhere in the body. Sometimes they are in specific areas, and sometimes they’re all over the place. Regardless, getting the drug to the target cells has always been a challenge. Our main delivery routes currently are swallowing, inhalation, skin absorption, and injection. Each has different uses, benefits, and drawbacks, but the route isn’t enough. Ingested medicines, for example, need to survive the harsh stomach acid but still be absorbable by the intestines. Injected medications are cleared by the liver at high speeds, reducing the effectiveness of a drug. Effective drug delivery means getting medicine to the right place at the right time, intact. One of the best-known developments in medications has been the use of mRNA in COVID vaccines. Actually getting the delicate molecules inside cells for an immune response was one of the unsung heroes of this vaccine. Scientists implemented lipid nanoparticles to get the job done. This was no easy challenge. Lipid nanoparticles are teeny packages of fat that protect the mRNA vaccine until it can get into target cells. They are small and strong to enter cells without disintegrating in the bloodstream. The development of lipid nanoparticles was just in time for the COVID pandemic and has shown to be very effective. The drawbacks are that they must be produced perfectly every time for billions of doses and must be kept extremely cold, at least currently. A much less widespread development has been the creation of microneedles. These are already in use for cosmeceutical applications. Microneedles are generally smaller than one or two millimeters and don’t puncture the skin all the way to the blood layer. This allows for simpler delivery and at-home administration of some medicines. Microneedles can also be coated with a dry version of medicines, allowing for shelf-stable drug delivery. This could be particularly helpful in areas with inadequate infrastructure and a lack of medical personnel. Researchers are developing many other new and exciting delivery methods. Targeted organ delivery is the practice of delivering medicine to specific organs. One example is coating a medicine in a urine-resistant coating for injection into the bladder. Cellular delivery uses living cells to carry medication to the target site. These living cells may be red blood cells or beneficial cyanobacteria. Attaching medicine to red blood cells can help drugs resist the powerful cleanup mechanism of the liver. This may allow for lower doses to have bigger effects. Attaching to beneficial spirulina platensis cyanobacteria may help medicines cross the stomach intact and deliver medicine straight to the intestines. This can allow for targeted organ delivery or for longer release of medicines. Finally, some scientists are experimenting with physically squeezing cells. This opens temporary pores for direct drug delivery. Such a system could enable scientists to deliver medicine to billions of cells per minute. All these exciting new delivery systems will have a big impact. Medicines of the future may be delivered in lower doses and with fewer side effects. We can also expect new uses for old medicines, as they will be able to be used in new ways and able to target new organs. Several of our clinical trials at Encore Research Group use these new methods. It’s an exciting time to help be on the cutting edge of what new medicine delivery will look like in the future. With luck, these new delivery methods will open new doors for medicines to help save lives and heal conditions. With even more luck, my buddy might get his bike by the end of the year. Written by: Benton Lowey-Ball, B.S. Behavioral Neuroscience
Sources: May, M. (2022). Why drug delivery is the key to new medicines. Nature Medicine, 28(6), 1100-1102. National Institute of Health, National Institute of Biomedical Imaging and Bioengineering. (October, 2016). Drug delivery systems. U.S. Department of Health and Human Services. https://www.nibib.nih.gov/science-education/science-topics/drug-delivery-systems-getting-drugs-their-targets-controlled-manner
Listen to the article here:
Ahoy ye mateys! Have you ever wondered which enemy was the most dangerous to sailors during the 1700’s? James Lind, a Royal Navy surgeon, described a foe which “proved a more destructive enemy, and cut off more valuable lives, than the united efforts of the French and Spanish arms.” In order to conquer this threat, Lind employed a brand new weapon. This weapon was previously unknown to science, and has now been used to defeat countless foes. The enemy was scurvy, and the weapon was a clinical trial. May 20, 2022 marks the 275th anniversary of that first clinical trial. Scurvy could lead to muscle pain, gum disease, fatigue, jaundice, and death. Remedies at the time varied widely and only anecdotal, word-of-mouth evidence for them was available. Every sailor who was afflicted with scurvy sought a cure, but the overall disease was caught in the doldrums without a solution for 150 years. Lind had bigger ambitions. His big insight wasn’t trying to treat just a few individuals for scurvy, but instead trying to solve the problem of scurvy on the scale of public health. Though he only had 12 participants in that first trial, how Lind compared different remedies showed his big-picture thinking. He sought not to give relief to just those 12 patients, but to quantify and share his results to cure the whole of the Royal Navy. In this effort Lind laid the groundwork of the modern clinical research study. He started with a set of 12 patients with conditions “as similar as I could have them.” He controlled extraneous variables, giving all patients the same diet during the study and keeping them on the same boat. He split them into 6 random conditions: The results were clear; citrus gave quick and significant relief. Importantly, Lind didn’t leave his findings high and dry. He recorded and reported what he saw. Probably the most important aspect of Lind’s clinical trial was that he looked at the results in an unbiased way. He wrote extensively on the need to remove personal and societal bias: “it is no easy matter to root out old prejudices, or to overturn opinions which have acquired an establishment of time, custom, and great authorities; it became therefore requisite for this purpose, to exhibit a full and impartial view of what has hitherto been published on scurvy.” Today the same core ideas guide clinical trials, but there are many more safeguards for participants. A good clinical trial today is grounded in science, provides benefits to patients that should outweigh any risks, and treats patients with respect. Critically, clinical trials have informed consent; all participants join voluntarily and must have full knowledge of any risks before signing up. Trials also have oversight from Institutional Review Boards and have medical staff on site to help with any adverse reactions. Following Lind’s example, clinical trials also target specific conditions, have randomized patients, control conditions (as much as possible), and dutifully record and report their findings. Though his aim was to blow scurvy out of the water, Lind ended up making waves in how scientists solve medical problems in general. His quantitative, balanced approach gave the world a system to tackle medical problems. On this International Clinical Trials Day we can help keep up the bounty of Lind’s legacy by volunteering as a clinical research trial participant and send some diseases to Davy Jones’ Locker! Written by Benton Lowey-Ball, BS Behavioral Neuroscience
Lind, J. (1753). A treatise of the scurvy: in three parts, containing an inquiry into the nature, causes, and cure, of that disease, together with a critical and chronological view of what has been published on the subject. Bulletin of the World Health Organization: the International Journal of Public Health 2004; 82 (10): 793-796.From https://www.jameslindlibrary.org/lind-j-1753/
Listen to the article here:
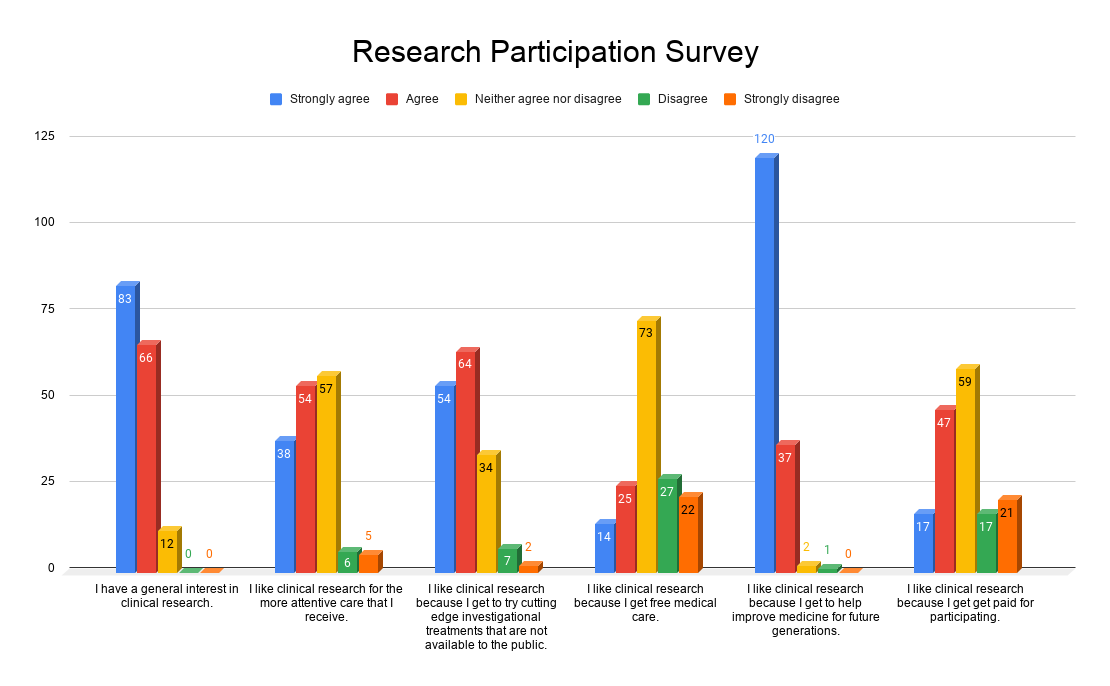
We asked, “What motivates you to participate in clinical trials?” With over 160 responses, the answer is clear. People who participate in clinical trials are dedicated to helping others by improving medicine for future generations.
We also found that very few were participating in order to receive the stipend for time and travel. This says a lot about the type of people who are willing to participate in clinical trials. They are in it for the cutting edge treatment, and the need to help others.
There is truly only one way to improve healthcare, and that is to participate in clinical trials. Thank you to everyone who responded to our survey, and everyone who participates in these trials.
On a sailing ship in 1747, twelve sailors who had begun the voyage feeling fine were overcome with fatigue. Their gums were swollen and sore, making it difficult to eat. Their teeth were falling out. Their legs were swollen and purple from bruising.
Dr. James Lind was a passenger on that ship, and he set out to find the cause. He set up what may have been the first clinical nutrition experiment. He decided on six groups of treatments, 2 sailors in each group:
- drank one quart of cider a day
- gargled with sulfuric acid
- had two spoonfuls of vinegar, 3 times a day
- drank ½ pint seawater a day
- drank barley water
- ate two oranges and 1 lemon a day
Within six days, the sailors who ate the oranges and lemon felt better and were able to work again. The other sailors in the experiment felt worse. The ill sailors were suffering from a lack of vitamin C, now known as Scurvy. They had plenty of fresh fruits and vegetables when they first set out on the voyage. But fresh foods ran out on the long voyage, and they suffered symptoms from this lack. After this finding, sailors often brought lime juice aboard ship because it could be stored longer. This is how sailors earned the nickname “limey”.
1747 was well before the requirement of informed consent of the patient, detailed eligibility criteria, protocols and regulations, which are a foundation of today’s clinical research. Nevertheless, it is an interesting example of a method of discovering the best treatment for a disabling condition.
Scientific minds are still seeking solutions for medical problems. Modern clinical research is strictly regulated for the safety and well-being of the research volunteer. Great progress has been made in medical science over the last decades. This progress could not happen without dedicated volunteers. Participation in clinical trials can be a rewarding endeavor for both investigators and volunteers alike.
Written by: Julia Baker, RN, CCRC
Resources:
https://askabiologist.asu.edu
https://www.umass.edu/nibble/infofile/limey.html
Thank You for a Great Year!
As an ENCORE community member, we hope you have enjoyed hearing from us this year. Each month we strive to provide you with accurate information on health topics that are relevant to you and our enrolling studies. 2018 has been a momentous year for us and has seen complete many trials for novel medications that we believe will improve global health. We are thankful for dedicated volunteers like you that make this possible!
This month we would like to do something a little different and provide you with insight into clinical trials. A lack of clinical trial education is routinely cited as the number one barrier to enrolling trial participants. Clinical trials are required by the FDA to prove the safety and effectiveness of new medications and volunteer participants are necessary to complete these trials. We understand that this concept is often intimidating. However, there are several measures in place to make our trials as safe as possible, including:
- Physicians in charge of all study activities
- Pre-Clinical Testing
- Institutional Review Boards (IRBs)
- Informed Consent Forms
- Routine Participant Labs and Clinical Assessments
- Clinical Trial Data Safety Monitoring Boards
Investigational products are thoroughly studied during pre-clinical testing before the trials are designed and the first human participant is enrolled. Pharmaceutical companies spend millions of dollars to bring medications to market and they want to be nearly certain that the medication will fulfill its intended purpose. However, volunteers are needed to complete the FDA clinical trials. When designing the trial protocols, participant safety is always the number one priority!
Every trial is overseen by an Institutional Review Board (IRB). The purpose of the IRB is to protect the rights and welfare of human research participants. The IRB evaluates the possible risks and benefits of the trial before it is allowed to open. They are also responsible for approving the trial protocol and the informed consent. Along with the consent form, a discussion with our medical staff allows you to make an informed decision on whether or not the trial is in your best interest. Lastly, participants in the study are continuously monitored for safety and there are many tests completed during the trials to alert researchers at the first sign of potentially serious side effects. We hope that every patient that has worked with us has felt that it has been a safe and positive experience!
Thank you again for helping us improve global health and find new ways to treat medical ailments! 2019 is going to be another exciting year at ENCORE Research and we hope to get the chance to work with everyone reading this letter.
Happy Holidays,
ENCORE Research
Why do our volunteers want to participate in clinical trials? Volunteers are often motivated by a combination of several reasons. Here are 6 of the top reasons to participate.
-
The potential of finding relief from their symptoms
We can’t promise relief from symptoms due to placebo and efficacy of the medication being tested. However, the Hawthorne Effect proves that patients who participate in a research trial have better outcomes than those not participating.
-
To learn more about their condition
You might argue that to learn about a condition you can just look it up on the web, and we all do that. However, often these websites can be misleading or provide the worst-case scenario results, which don’t apply to most of us. Another option is to ask your primary physician, and that is a good thing to do. Unfortunately, physicians are often rushed or running behind and questions are forgotten. Participating in a clinical trial provides you ample one on one time with a research professional and physician so that all your questions can be answered.
-
Access to new cutting-edge treatments
When participating in a clinical trial, there is access to new cutting edge treatments that are not available yet to the public. There can even be access to medications that have been newly FDA approved, but are much too expensive to afford. Study required medications are most often provided at no cost!
-
Receiving medical care at no cost
Sponsors such as pharmaceutical companies, governments and foundations fund medical research through study grants. The grants fund local research sites for conducting the study so you don’t pay a thing. In fact, we don’t even ask you for your insurance information! Can you believe most studies compensate patients for time and travel?
-
Making a difference
Clinical Trials help shape the future of medicine and healthcare. Volunteer participation helps researchers discover more about health conditions and find better ways to treat them!
-
Moral and emotional support
Having medical conditions that others don’t necessarily understand can make some people feel alienated. When involved in research, support staff understand the patient’s condition and what they may be experiencing and can provide moral and emotional support.
We will do everything we can to help find a trial that is a good fit for interested volunteers. New clinical trials are constantly enrolling so do not be discouraged if we don’t currently have the perfect trial for you. The majority of volunteers who completed a clinical trial are interested in participating in another one, so call us and find out your reason to participate!
At ENCORE Research Group it is our mission to help every patient that walks through our doors qualify for the clinical trial of their choice. Often times we get to experience the thrill of telling our patients that they successfully qualified and will soon enroll in the study. However, this is not always the case and we understand our patients’ frustration when they decide to commit to a trial only to later find out that they do not qualify. Here at ENCORE Research Group we were curious how this situation affected their thoughts about applying for future studies. This month, curiosity got the best of us and we reached out to some of our community members to find out!
Thomas recently came to Jacksonville Center for Clinical Research (JCCR) to have an evaluation for a high triglyceride and weight loss study. Fortunately for Thomas, he was not eligible for the trial because his triglyceride level was too low. Thomas stated “it’s good that I am healthy enough not to be in this research study. But they are looking at another study that I may be interested in.” As you can see, Thomas was not discouraged that he did not qualify, but optimistic that he may qualify for a different study.
We also reached out to Latasha, who is new to research, and may qualify for a study that has a waiting list for interested participants. When discussing with her how some patients are not eligible to join a trial, she stated “I would want to know why I did not qualify, but that would not prevent me from trying to get in another trial.” Fortunately for Latasha and all of our participants, ENCORE Research Group is very transparent about the screening process and explains exactly why they may have been ineligible. Hopefully she will receive a spot in the study she applied for!
Mark was passionate about participating in a Sjogren’s research trial but did not qualify. He said “it’s not unusual for someone with Sjogren’s Disease not to qualify for studies with systemic therapies if they do not have the antibodies. But when you’re sick, your driving force is to get better for yourself and your family. I tried the conventional way but it did not work for me.” After doing more research on the specific clinical trial, Mark decided to pursue the FDA Expanded Access program. “It’s a relatively new program to help people get access to new medications.” Fortunately for Mark, he had the resources and insight to look into alternative treatment options.
We also asked an experienced researcher how she saw things. Linda Gray, site manager of the Nature Coast Clinical Research site in Inverness, Florida, has many gastrointestinal (GI) studies currently enrolling. Linda acknowledges that “some of our patients are not eligible for a study because they have mild disease, and the sponsors are looking for moderate to severe disease. If the disease is not measurable enough for objective data, we will not be able to tell if we’ve reversed it or slowed the progression. Our NASH studies include a liver biopsy to determine the extent of the disease to see if the patient is eligible.” It is unfortunate that this can limit access to drugs for those in need, but we have to believe that obtaining clear and objective data will help a greater number of people in the future.
The reality is, every clinical trial is different and has unique qualifying criteria. The pharmaceutical companies that sponsor clinical trials create the criteria in order to make the strongest case possible to the FDA on the drug’s safety and efficacy. While we would love to involve every one of our community members that are interested, it is just not always possible. The good news is that all seven of our research sites are always getting new clinical trials to enroll in! So, just because you didn’t qualify the first time doesn’t mean you won’t qualify for the next one! We look forward to working with you in the ENCORE community.
The practice of medicine has changed in major ways in recent years. Though many of these changes reflect good intentions, the real world consequences to patients often don’t match expectations. To understand this divide between reasonable intentions and the less salubrious reality from which we may collectively suffer, I’d like to share a recent anecdote that occurred at the airport when regulations ran amok.
During recent travel, I witnessed an unfortunate incident that you may have seen before. An airline gate agent stopped a member of our party and reprimanded her for carrying a small overnight suitcase, a computer bag and her pocketbook. The gate agent, working on behalf of the airline, stated that she had to follow FAA (Federal Aviation Authority) rules and only allow two bags on board even though the computer bag and pocket book were small. Unfortunately, when asked to “consolidate” the three bags into two, we had a problem. No bag really fit into any of the other bags. The agent wouldn’t “gate check” any of the bags so that we could pick it up when exiting the plane and running off to our next flight. Further, our discussion with the gate agent failed to alleviate our concern that, if checked to its “final destination,” we wouldn’t see a checked piece of luggage any time soon given the shortness of time for our connection.
The solution that followed satisfied no one. Over the next 10 minutes, embarking passengers stepped around the contents of the three bags which littered the entrance to the Jetway. At first, the gate agents ignored the situation, but as tempers flared due to the obstruction of foot traffic, an agent “helped” by aggressively stuffing the computer bag into the overnight bag. A busted zipper later, the bulging overnight bag limped down the Jetway led by a very unhappy customer.
Does this scenario prove airline excellence because the agents showed how well they can comply with government rules? Hardly! Most folks would conclude that this messy scenario wasn’t necessary. In complex situations, the empowerment of professionals to act judiciously given a set of circumstances leads to excellence. The above scenario required the gate agents to apply context while making an overall effort to comply with government regulations. Unfortunately an excellent result didn’t happen in this case.
Similarly, we face the issue of context and judicious interpretation every day in medicine. As a common example, computerized medical records, a well-intended effort to characterize complex information, often fail to convey the true story of a patient or the nuances that make each of us unique. Summarized, bullet point information can easily miss the point. The great composer Mozart famously observed that musical excellence doesn’t lie in the notes but actually in the space and timing in between the sounds. Medical excellence involves a similar concept. Health care providers must read “in between the lines” and understand and respond both to what is and isn’t stated.
What this concept means to the average patient depends on the circumstances. For example, some people with neck pain may need consideration for a heart condition (angina) whereas others should check in immediately for an MRI of the spine and others should book a massage. Distinguishing the underlying cause of the neck pain relies on both a description of the nature of the symptom and on understanding the quiescent pauses of relief between episodes of pain. Excellent clinicians make this distinction by asking the right questions. Excellence during the medical evaluations of headaches, arthritis, and memory problems, among other things, also require this same commitment to careful questioning.
Clinical research promotes excellence by demanding great attention to detail. During research programs, physician investigators and their staff members must extensively analyze many aspects of our patients’ health. This thorough analysis usually exceeds that which occurs at the time of general physician visits, a setting during which time pressed clinicians must limit their focus and move on to the next patient. Research also requires the deployment of state of the art technology. The combination of technology and attention to detail of symptoms, signs and lab values leads to an experience which most patients highly value and describe as a demonstration of medical excellence.
In sum, medical excellence involves more than compliance or automatically matching a disease with a drug. Medical excellence is a philosophy of understanding the needs of a patient and putting those needs in context through the development of an individual treatment plan. Clinical research promotes medical excellence by demanding a culture of detail and caring.
Let’s not dance around the issue: for many years now, news sources like CBS, CNN, The Atlantic, and The New Yorker have called research volunteers guinea pigs. You’ve probably said it yourself. I’m here today to tell you why we need to call research volunteers by another name: Heroes.
The term “guinea pig” is condescending to both volunteers and researchers. For volunteers, it takes away the enormity of their contribution by sounding like they have no choice in the matter. If you have ever taken a prescription medicine for any reason, even an antibiotic; someone has chosen to volunteer to make sure the medicine is safe and works. If medicines down the road are to work better, we need volunteers to keep agreeing to test them.
Calling subjects “guinea pigs” also disdains the research coordinators and doctors that supervise drugs trials. Before any volunteer is admitted into a trial, coordinators fully explain what the trial entails, making sure to answer any questions or concerns of the volunteer. If the volunteer agrees, they go through a screening process to make sure they are a good fit for the trial and that the trial is safe for them. During the trial, the volunteer tells the coordinator or doctor about any medical events, including colds, broken toes, or headaches. This is also for safety, and if anything happens, the volunteer is free to stop the study or change their mind about participating. Throughout the study, the volunteer’s health is closely monitored; patient safety is always first. If a volunteer decides they no longer want to be in a clinical trial, they can withdraw from the trial at any time and will not be coerced to stay.
Before any medicine hits the market it is tested for years, with data constantly being reviewed in between trials. New medicines will go through 3 – 4 clinical trials over many years, with safety and effectiveness being the top concerns.
So, why are volunteers not guinea pigs? Guinea pigs (or any animal for that matter) don’t willingly sign up to be a part of future healthcare that could save lives. Guinea pigs are cute, fat, fuzzy, and they eat their own poop (Coprophagy). But, they do not willingly agree to be part of a trial that could save lives down the road.
So I urge you, quit using the term guinea pig for volunteers, use the term hero instead! We can’t cure diseases without heroes.
If you have volunteered for a clinical trial before, YOU ARE A HERO! If you have never participated, become a research HERO today!
Recently, I had my first experience as a clinical research volunteer. Going in, I wasn’t quite sure what to expect, but it was better than I thought!
I have Multiple Sclerosis. I also have asthma, arthritis, hypothyroidism, high blood pressure, and migraines. I live with chronic pain, I’ve had multiple surgeries, and the list goes on. With all these illnesses and conditions I need prescription medications to function on a daily basis.
I’m your average Google symptoms and side effects checker. I think it’s very important since I’m on over 10 daily medications to treat my health issues. I see multiple specialists; and I can’t expect them to research and remember all the ways those medicines interact with the others I’m already on. So I try to be smart about it.
Being a research volunteer has some bad stigmas attached to it. Some people think you might grow a second head or something! I’m here to tell you, don’t believe those outlandish tales! Without volunteers like me, the drugs I’m taking that stop horrible leg cramps or make my migraines back off- wouldn’t have made it to the pharmacy shelves.
When a friend of mine mentioned that her daughter works at Jacksonville Center for Clinical Research, for some reason that statement humanized the whole idea of prescription medications for me.
So I googled them and found they had SO many opportunities for many of the medical problems I currently have. I filled out an online form to be contacted, and a bubbly, friendly lady called me. I wasn’t even sure what to say but she dove right in talking about the different issues I mentioned on the form. She gave me an idea of what they were looking for in the studies, and I answered her questions. It was easy. In no time she had singled out a study I might be perfect for and set up an appointment. We talked through most of it over the telephone and she had it all together when I arrived. It turned out I WAS the perfect fit. It was a study that only required me to come to 3 appointments over a 6 week period and paid me $400. Wow! Did that extra cash come in handy! While I was there everyone treated me like an old friend.
I am doing my part to help put good drugs on the shelves for myself and millions of other people.
Now I know what it’s like to be a hero.
Tracy
THE RESULTS ARE IN!
We would like to wish a big heartfelt THANK YOU to all our volunteers that participated in this international (PCSK9) high cholesterol study of 1300 volunteers completed in 18 countries.
Jacksonville FL volunteers lead the world in this study with ground breaking results! Our own CEO Dr. Michael J. Koren was the lead international investigator and lead author on the study. Results published in Jama Cardiology.